An evaluation of three-dimensional facial changes after surgically assisted rapid maxillary expansion (SARME): an observational study
- PMID: 35501780
- PMCID: PMC9063160
- DOI: 10.1186/s12903-022-02179-1
An evaluation of three-dimensional facial changes after surgically assisted rapid maxillary expansion (SARME): an observational study
Abstract
Background: The abnormal facial features in maxillary transverse deficiency (MTD) are minimal and limited to a deficiency of the middle facial third, narrow nares and nasal base, and deepened nasolabial folds. The surgical expansion of the narrow maxilla has most obvious effects on widening of the maxillary dental arch and expansion of the maxillary and palatal structures in the transverse plane, however sagittal changes also occurs. The purpose of this observational study was to evaluate the three-dimensional (3D) facial soft tissue changes following surgically assisted rapid maxillary expansion (SARME).
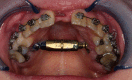
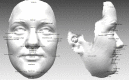
Methods: In 15 skeletally mature patients with severe maxillary transverse deficiency, the planned maxillary expansion (on average 8.8 mm ± 2.3 mm) was achieved with a bone-borne palatal distractor. The 3D optical scans of the facial surface were obtained before and six months after SARME. In the first part, we defined different anatomical landmarks on both scans and compared cephalometric measurements. In the second part, we registered both 3D scans in the same workplace using the regional best-fit method (forehead, supraorbital and nasal root regions were selected for the superimposition) and conducted surface analysis.
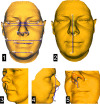
Results: The largest differences between the pre- and post-operation scans were observed in the paranasal and cheek area (1.4 ± 1.0 mm). Significant differences occurred for an increased nasal width, a decreased upper-face height with an unchanged lower height, an increased vertical philtrum height and an increased nasolabial angle. A significant increase in the facial profile angle was also observed, resulting in an increased facial convexity and anterior displacement of the upper-lip area.
Conclusions: The widening of the nose and increased projection in the cheek and paranasal area in the lateral direction after maxillary expansion were confirmed; moreover, facial convexity increases, reflecting the underlying advancement of the maxilla.
Keywords: 3D scanning; Facial scan; Facial soft tissue; Maxillary expansion; Maxillary osteotomy.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures



References
-
- Betts NJ, Vanarsdall RL, Barber HD, Higgins-Barber K, Fonseca RJ. Diagnosis and treatment of transverse maxillary deficiency. Int J Adult Orthodon Orthognath Surg. 1995;10(2):75–96. - PubMed
-
- Tosa H, Imai T, Watanabe F, Sumori M, Tsuchida T, Matsuno I, et al. The clinical study on occurrence of TMJ dysfunction in orthodontic patients. Nippon Kyosei Shika Gakkai Zasshi. 1990;49(4):341–351. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

