Long-term mortality following SARS-CoV-2 infection: A national cohort study from Estonia
- PMID: 35505834
- PMCID: PMC9051903
- DOI: 10.1016/j.lanepe.2022.100394
Long-term mortality following SARS-CoV-2 infection: A national cohort study from Estonia
Abstract
Background: The objective of this study was to describe 12-month mortality following SARS-CoV-2 infection compared with a reference population with no history of SARS-CoV-2.
Methods: Nationwide cohort study using electronic health care data on SARS-CoV-2 RNA positive cases (n= 66,287) and reference group subjects (n=254,969) with linkage to SARS-CoV-2 testing and death records.
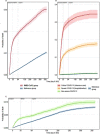
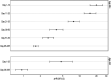
Findings: People infected with SARS-COV-2 had more than three times the risk of dying over the following year compared with those who remained uninfected (aHR 3·1, 95%CI 2·9-3·3). Short-term mortality (up to 5 weeks post-infection) was significantly higher among COVID-19 group (1623·0/10 000) than in the reference group (118/10 000). For COVID-19 cases aged 60 years or older, increased mortality persisted until the end of the first year after infection, and was related to increased risk for cardiovascular (aHR 2·1, 95%CI 1·8-2·3), cancer (aHR 1·5, 95%CI 1·2-1·9), respiratory system diseases (aHR 1·9, 95%CI 1·2-3·0), and other causes of death (aHR 1·8, 95%CI 1·4-2·2).
Interpretation: Increased risk of death from SARS-CoV-2 is not limited to the acute illness: SARS-CoV-2 infection carries a substantially increased mortality in the following 12 months. This excess death mainly occurs in older people and is driven by broad array of causes of death.
Funding: Research was carried out with the support of Estonian Research Council (grants PRG1197, PRG198), European Regional Development Fund (RITA 1/02-120) and European Social Fund via IT Academy program.
Keywords: COVID-19; Cardiovascular death; Estonia; Mortality; Population-based; SARS-CoV-2.
© 2022 The Author(s).
Conflict of interest statement
The authors report no conflicts of interest.
Figures


References
-
- Al-Aly Z, Xie Y, Bowe B. High-dimensional characterization of post-acute sequelae of COVID-19. Nature. 2021;594:259–264. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

