Using a daily monitoring system to reduce treatment position override rates in external beam radiation therapy
- PMID: 35506575
- PMCID: PMC9278683
- DOI: 10.1002/acm2.13629
Using a daily monitoring system to reduce treatment position override rates in external beam radiation therapy
Abstract
Purpose/objectives: To report our 7-year experience with a daily monitoring system to significantly reduce couch position overrides and errors in patient treatment positioning.
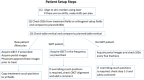
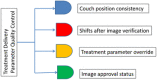
Materials and methods: Treatment couch position override data were extracted from a radiation oncology-specific electronic medical record system from 2012 to 2018. During this period, we took several actions to reduce couch position overrides, including reducing the number of tolerance tables from 18 to 6, tightening tolerance limits, enforcing time outs, documenting reasons for overrides, and timely reviewing of overrides made from previous treatment day. The tolerance tables included treatment categories for head and neck (HN) (with/without cone beam CT [CBCT]), body (with/without CBCT), stereotactic body radiotherapy (SBRT), and clinical setup for electron beams. For the same time period, we also reported treatment positioning-related incidents that were recorded in our departmental incident report system. To verify our tolerance limits, we further examined couch shifts after daily kilovoltage CBCT (kV-CBCT) for the patients treated from 2018 to 2021.
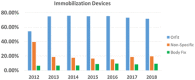
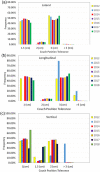
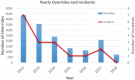
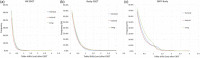
Results: From 2012 to 2018, the override rate decreased from 11.2% to 1.6%/year, whereas the number of fractions treated in the department increased by 23%. The annual patient positioning error rate was also reduced from 0.019% in 2012, to 0.004% in 2017 and 0% in 2018. For patients treated under daily kV-CBCT guidance from 2018 to 2021, the applied couch shifts after imaging registration that exceeded the tolerance limits were low, <1% for HN, <1.2% for body, and <2.6% for SBRT.
Conclusions: The daily monitoring system, which enables a timely review of overrides, significantly reduced the number of treatment couch position overrides and ultimately resulted in a decrease in treatment positioning errors. For patients treated with daily kV-CBCT guidance, couch position shifts after CBCT image guidance demonstrated a low rate of exceeding the set tolerance.
Keywords: automation; external beam radiotherapy; patient safety; treatment couch overrides; treatment positioning errors.
© 2022 The Authors. Journal of Applied Clinical Medical Physics published by Wiley Periodicals, LLC on behalf of The American Association of Physicists in Medicine.
Conflict of interest statement
No conflict interest is related to this manuscript.
Figures
References
-
- Bogdanich W. As technology surges, radiation safeguards lag. The New York Times Inc. 2010.
-
- Bogdanich W. The radiation boom: radiation offers new cures, and ways to do harm. New York Times. January 23, 2010. section A:1.
-
- Chang DW, Cheetham L, te Marvelde L, et al. Risk factors for radiotherapy incidents and impact of an online electronic reporting system. Radiother Oncol. 2014;112(2):199–204. - PubMed
-
- Elnahal SM, Blackford A, Smith K, et al. Identifying predictive factors for incident reports in patients receiving radiation therapy. Int J Radiat Oncol Biol Phys. 2016;94(5):993–999. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

