Effect of Pore Size of Porous-Structured Titanium Implants on Tendon Ingrowth
- PMID: 35510044
- PMCID: PMC9061050
- DOI: 10.1155/2022/2801229
Effect of Pore Size of Porous-Structured Titanium Implants on Tendon Ingrowth
Abstract
Purpose: The reconstruction of a tendon insertion on metal prostheses is a challenge in orthopedics. Of the available metal prostheses, porous metal prostheses have been shown to have better biocompatibility for tissue integration. Therefore, this study is aimed at identifying an appropriate porous structure for the reconstruction of a tendon insertion on metal prostheses.
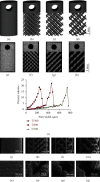
Methods: Ti6Al4V specimens with a diamond-like porous structure with triply periodic minimal surface pore sizes of 300, 500, and 700 μm and a porosity of 58% (designated Ti300, Ti500, and Ti700, respectively) were manufactured by selective laser melting and were characterized with micro-CT and scanning electron microscopy for their porosity, pore size, and surface topography. The porous specimens were implanted into the patellar tendon of rabbits. Tendon integration was evaluated after implantation into the tendon at 4, 8, and 12 weeks by histology, and the fixation strength was evaluated with a pull-out test at week 12.
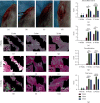
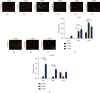
Results: The average pore sizes of the Ti300, Ti500, and Ti700 implants were 261, 480, and 668 μm, respectively. The Ti500 and Ti700 implants demonstrated better tissue growth than the Ti300 implant at weeks 4, 8, and 12. At week 12, the histological score of the Ti500 implant was 13.67 ± 0.58, and it had an area percentage of type I collagen of 63.90% ± 3.41%; both of these results were significantly higher than those for the Ti300 and Ti700 implants. The pull-out load at week 12 was also the highest in the Ti500 group.
Conclusion: Ti6Al4V implants with a diamond-like porous structure with triply periodic minimal surface pore size of 500 μm are suitable for tendon integration.
Copyright © 2022 Yupeng Guo et al.
Conflict of interest statement
The authors declare that they have no conflicts of interest.
Figures

References
LinkOut - more resources
Full Text Sources

