The effect of integrated health care in patients with hypertension and diabetes: a systematic review and meta-analysis
- PMID: 35513809
- PMCID: PMC9074341
- DOI: 10.1186/s12913-022-07838-1
The effect of integrated health care in patients with hypertension and diabetes: a systematic review and meta-analysis
Abstract
Background: A growing number of studies show that integrated health care provides comprehensive and continuous care to patients with hypertension or diabetes. However, there is still no consensus about the effect of integrated health care on patients with hypertension or diabetes. The objective of this study was to verify the effectiveness of integrated health care for patients with hypertension or diabetes by using a systematic review and meta-analysis.
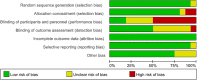
Methods: The study searched multiple English and Chinese electronic databases. The search period was from database inception to 31 October 2020. Systematic reviews and meta-analyses were conducted after assessing the risk of bias of each study.
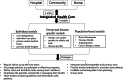
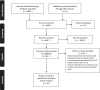
Results: Sixteen studies that involved 5231 patients were included in this study. The results of the systematic review revealed that systolic blood pressure (SBP), diastolic blood pressure (DBP), body mass index (BMI) and glycosylated haemoglobin (HbA1c) are commonly used indicators for patients with hypertension or diabetes. Individual models and group- and disease-specific models are the most commonly used models of integrated health care. All the studies were from high-income and middle-income countries. Meta-analysis showed that integrated health care significantly improved SBP, DBP and HbA1c but not BMI. A comparison of interventions lasting 6 and 12 months for diabetes was conducted, and HbA1c was decreased after 12 months. The changes in SBP and DBP were statistically significant after using group- and disease-specific model but not individual models. HbA1c was significantly improved after using group- and disease-specific models and individual models.
Conclusion: Integrated health care is a useful tool for disease management, and individual models and group- and disease-specific models are the most commonly used models in integrated health care. Group- and disease-specific models are more effective than individual models in the disease management of hypertension patients. The duration of intervention should be considered in the disease management of patients with diabetes, and interventions longer than 12 months are recommended. The income level may affect the model of integrated health care in selecting which disease to intervene, but this point still needs support from more studies.
Keywords: Diabetes; Hypertension; Integrated health care; Meta-analysis; Systematic review.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures






References
-
- Xu J, Yang F, Si L, Qian D. Do integrated health care interventions improve well-being among older adults with hypertension? Evidence from rural China. Social Indicators Research. 2022;160:825–843. doi: 10.1007/s11205-020-02482-w. - DOI
-
- Organization WH . WHO global strategy on people-centred and integrated health services: interim report. World Health Organization; 2015.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

