Automated quantitative assessment of amorphous calcifications: Towards improved malignancy risk stratification
- PMID: 35525068
- PMCID: PMC9839357
- DOI: 10.1016/j.compbiomed.2022.105504
Automated quantitative assessment of amorphous calcifications: Towards improved malignancy risk stratification
Abstract
Background: Amorphous calcifications noted on mammograms (i.e., small and indistinct calcifications that are difficult to characterize) are associated with high diagnostic uncertainty, often leading to biopsies. Yet, only 20% of biopsied amorphous calcifications are cancer. We present a quantitative approach for distinguishing between benign and actionable (high-risk and malignant) amorphous calcifications using a combination of local textures, global spatial relationships, and interpretable handcrafted expert features.
Method: Our approach was trained and validated on a set of 168 2D full-field digital mammography exams (248 images) from 168 patients. Within these 248 images, we identified 276 image regions with segmented amorphous calcifications and a biopsy-confirmed diagnosis. A set of local (radiomic and region measurements) and global features (distribution and expert-defined) were extracted from each image. Local features were grouped using an unsupervised k-means clustering algorithm. All global features were concatenated with clustered local features and used to train a LightGBM classifier to distinguish benign from actionable cases.
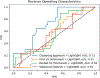
Results: On the held-out test set of 60 images, our approach achieved a sensitivity of 100%, specificity of 35%, and a positive predictive value of 38% when the decision threshold was set to 0.4. Given that all of the images in our test set resulted in a recommendation of a biopsy, the use of our algorithm would have identified 15 images (25%) that were benign, potentially reducing the number of breast biopsies.
Conclusions: Quantitative analysis of full-field digital mammograms can extract subtle shape, texture, and distribution features that may help to distinguish between benign and actionable amorphous calcifications.
Keywords: Machine learning; Mammography; Microcalcifications; Radiomics.
Copyright © 2022 The Authors. Published by Elsevier Ltd.. All rights reserved.
Figures
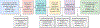
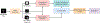


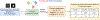
References
-
- Bassett LW, Lee-Felker S, 26 - breast imaging screening and diagnosis, in: Bland K, Copeland EM, Klimberg VS, Gradishar WJ (Eds.), Breast Fifth, Elsevier, 2018, 337–361.e2.
-
- Lee AY, Wisner DJ, Aminololama-Shakeri S, Arasu VA, Feig SA, Hargreaves J, et al. , Inter-reader variability in the use of BI-rads descriptors for suspicious findings on diagnostic mammography: a multi-institution study of 10 academic radiologists, Acad. Radiol 24 (2017) 60–66, 10.1016/j.acra.2016.09.010. - DOI - PubMed

