Impact of Body Mass Index on Survival Outcomes of Patients with Metastatic Renal Cell Carcinoma in the Immuno-oncology Era: A Systematic Review and Meta-analysis
- PMID: 35528786
- PMCID: PMC9068728
- DOI: 10.1016/j.euros.2022.03.002
Impact of Body Mass Index on Survival Outcomes of Patients with Metastatic Renal Cell Carcinoma in the Immuno-oncology Era: A Systematic Review and Meta-analysis
Erratum in
-
Corrigendum re "Impact of Body Mass Index on Survival Outcomes for Patients with Metastatic Renal Cell Carcinoma in the Immuno-oncology Era: A Systematic Review and Meta-analysis" [Eur Urol Open Sci 2022;39:62-71].Eur Urol Open Sci. 2022 Dec 19;48:17. doi: 10.1016/j.euros.2022.12.001. eCollection 2023 Feb. Eur Urol Open Sci. 2022. PMID: 36583180 Free PMC article.
Abstract
Context: Body mass index (BMI) is a useful tool for measuring body composition. It is unclear whether high BMI is a favourable indicator in patients with metastatic renal cell carcinoma (mRCC) treated with immune checkpoint inhibitors (ICIs).
Objective: To investigate the prognostic significance of BMI in patients with mRCC treated with ICIs in a systematic review and meta-analysis.
Evidence acquisition: Ovid MEDLINE, Embase, and Web of Science were systematically searched in July 2021, and meta-analysis was performed in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement.
Evidence synthesis: A total of 517 nonduplicate citations were screened by title and abstract, followed by full-text screening of 57 candidate articles to determine whether each study met the eligibility criteria. Overall, a total of 2281 patients from eight studies were included in the systematic review and meta-analysis. BMI levels were compared with overall survival (OS) and progression-free survival (PFS) in seven and three studies, respectively. Overweight/obese BMI was significantly associated with better OS compared to normal BMI (adjusted hazard ratio [aHR] 0.77, 95% confidence intervals [CI] 0.65-0.91; p = 0.002). A similar trend was observed for PFS (aHR 0.66, 95% CI 0.44-1.00; p = 0.050). There was no statistical heterogeneity or obvious publication bias among these studies.
Conclusions: This is the first systematic review and meta-analysis to evaluate the impact of BMI on survival outcomes of patients with mRCC treated with ICIs. To confirm the existence of the obesity paradox for patients with mRCC in the immuno-oncology era, high-quality clinical trials and basic research are warranted.
Patient summary: We reviewed published data on survival outcomes of 2281 patients with metastatic kidney cancer treated with immunotherapy drugs in relation to their body mass index (BMI). We found that higher BMI was associated with better survival when compared to normal BMI for this disease setting and treatment strategy.
Keywords: Body mass index; Immune checkpoint inhibitors; Meta-analysis; Obesity; Prognosis; Renal cell carcinoma.
© 2022 The Author(s).
Figures
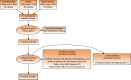


References
-
- Scelo G., Larose T.L. Epidemiology and risk factors for kidney cancer. J Clin Oncol. 2018;36:3574–3581.
-
- Bagheri M., Speakman J.R., Shemirani F., Djafarian K. Renal cell carcinoma survival and body mass index: a dose-response meta-analysis reveals another potential paradox within a paradox. Int J Obes. 2016;40:1817–1822.
-
- Kim L.H., Doan P., He Y., Lau H.M., Pleass H., Patel M.I. A systematic review and meta-analysis of the significance of body mass index on kidney cancer outcomes. J Urol. 2021;205:346–355. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

