Glutaminolysis-ammonia-urea Cycle Axis, Non-alcoholic Fatty Liver Disease Progression and Development of Novel Therapies
- PMID: 35528989
- PMCID: PMC9039703
- DOI: 10.14218/JCTH.2021.00247
Glutaminolysis-ammonia-urea Cycle Axis, Non-alcoholic Fatty Liver Disease Progression and Development of Novel Therapies
Abstract
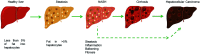
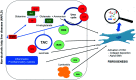
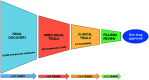
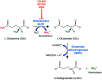
The prevalence of non-alcoholic fatty liver disease (NAFLD) is increasing worldwide, reflecting the current epidemics of obesity, insulin resistance, type 2 diabetes mellitus, and metabolic syndrome. NAFLD is characterized by the accumulation of fat in the liver, and is known to be a cause of cirrhosis. Although many pathways have been proposed, the cause of NAFLD-linked fibrosis progression is still unclear, which posed challenges for the development of new therapies to prevent NASH-related cirrhosis and hepatocellular carcinoma. Cirrhosis is associated with activation of hepatic stellate cells (HSC) and accumulation of excess extracellular matrix proteins, and inhibiting the activation of HSCs would be expected to slow the progression of NAFLD-cirrhosis. Multiple molecular signals and pathways such as oxidative stress and glutaminolysis have been reported to promote HSC activation. Both mechanisms are plausible antifibrotic targets in NASH, as the activation of HSCs the proliferation of myofibroblasts depend on those processes. This review summarizes the role of the glutaminolysis-ammonia-urea cycle axis in the context of NAFLD progression, and shows how the axis could be a novel therapeutic target.
Keywords: Ammonia; Cirrhosis; Fibrosis; Glutaminolysis; Non-alcoholic fatty liver disease; Urea.
© 2022 Authors.
Conflict of interest statement
The authors have no conflict of interests related to this publication.
Figures
Similar articles
-
Ammonia: A novel target for the treatment of non-alcoholic steatohepatitis.Med Hypotheses. 2018 Apr;113:91-97. doi: 10.1016/j.mehy.2018.02.010. Epub 2018 Feb 15. Med Hypotheses. 2018. PMID: 29523305
-
Macrophage-derived thrombospondin 1 promotes obesity-associated non-alcoholic fatty liver disease.JHEP Rep. 2020 Oct 9;3(1):100193. doi: 10.1016/j.jhepr.2020.100193. eCollection 2021 Feb. JHEP Rep. 2020. PMID: 33294831 Free PMC article.
-
Emerging and Established Therapeutic Approaches for Nonalcoholic Fatty Liver Disease.Clin Ther. 2021 Sep;43(9):1476-1504. doi: 10.1016/j.clinthera.2021.07.013. Epub 2021 Aug 24. Clin Ther. 2021. PMID: 34446271 Review.
-
Hedgehog-YAP Signaling Pathway Regulates Glutaminolysis to Control Activation of Hepatic Stellate Cells.Gastroenterology. 2018 Apr;154(5):1465-1479.e13. doi: 10.1053/j.gastro.2017.12.022. Epub 2018 Jan 3. Gastroenterology. 2018. PMID: 29305935 Free PMC article.
-
The Role of Insulin Resistance and Diabetes in Nonalcoholic Fatty Liver Disease.Int J Mol Sci. 2020 May 29;21(11):3863. doi: 10.3390/ijms21113863. Int J Mol Sci. 2020. PMID: 32485838 Free PMC article. Review.
Cited by
-
Understanding gut-liver axis nitrogen metabolism in Fatty Liver Disease.Front Endocrinol (Lausanne). 2022 Dec 15;13:1058101. doi: 10.3389/fendo.2022.1058101. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 36589817 Free PMC article. Review.
-
Ammonia scavenger and glutamine synthetase inhibitors cocktail in targeting mTOR/β-catenin and MMP-14 for nitrogen homeostasis and liver cancer.Med Oncol. 2023 Dec 29;41(1):38. doi: 10.1007/s12032-023-02250-z. Med Oncol. 2023. PMID: 38157146
-
Partially replacing dietary starch with soybean oil improved production performance of weaned Rex rabbits.J Anim Sci. 2025 Jan 4;103:skae381. doi: 10.1093/jas/skae381. J Anim Sci. 2025. PMID: 39693353
-
Ammonia-induced stress response in liver disease progression and hepatic encephalopathy.Nat Rev Gastroenterol Hepatol. 2024 Nov;21(11):774-791. doi: 10.1038/s41575-024-00970-9. Epub 2024 Sep 9. Nat Rev Gastroenterol Hepatol. 2024. PMID: 39251708 Review.
