Incorporating Blood Flow in Nerve Injury and Regeneration Assessment
- PMID: 35529911
- PMCID: PMC9069240
- DOI: 10.3389/fsurg.2022.862478
Incorporating Blood Flow in Nerve Injury and Regeneration Assessment
Abstract
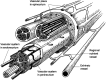
Peripheral nerve injury is a significant public health challenge, with limited treatment options and potential lifelong impact on function. More than just an intrinsic part of nerve anatomy, the vascular network of nerves impact regeneration, including perfusion for metabolic demands, appropriate signaling and growth factors, and structural scaffolding for Schwann cell and axonal migration. However, the established nerve injury classification paradigm proposed by Sydney Sunderland in 1951 is based solely on hierarchical disruption to gross anatomical nerve structures and lacks further information regarding the state of cellular, metabolic, or inflammatory processes that are critical in determining regenerative outcomes. This review covers the anatomical structure of nerve-associated vasculature, and describes the biological processes that makes these vessels critical to successful end-organ reinnervation after severe nerve injuries. We then propose a theoretical framework that incorporates measurements of blood vessel perfusion and inflammation to unify perspectives on all mechanisms of nerve injury.
Keywords: Sunderland injury classification; blood vessel; nerve injury; perfusion; peripheral nerve; regeneration.
Copyright © 2022 Yeoh, Warner, Merchant, Hsu, Agoston and Mahan.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


References
Publication types
LinkOut - more resources
Full Text Sources

