Comparison of 3D printed anatomical model qualities in acetabular fracture representation
- PMID: 35530954
- PMCID: PMC9073767
- DOI: 10.21037/atm-21-5069
Comparison of 3D printed anatomical model qualities in acetabular fracture representation
Abstract
Background: Acetabular fractures account for 10% of pelvis injuries, which are especially difficult to treat in developing countries with less access to resources. 3D printing has previously been shown to be a beneficial method of surgical planning, however the steep initial costs associated with purchasing a 3D printer may prevent some facilities form utilizing this technique. The purpose of this study was to develop 3D printed models for acetabular surgery using methodologies of varying cost to determine differences in model accuracy and overall quality.
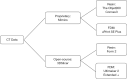
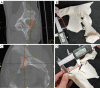
Methods: Five acetabular fracture models were developed from de-identified CT data using (I) proprietary and open-source segmentation software and (II) fused deposition modeling (FDM) and stereolithography (SLA) 3D printing methods. The distance between the posterior inferior iliac spine (PIIS) and the ischial spine as well as a unique fracture fragment for each model was compared between the different printing methodologies. The models were then given to 5 physicians and assessed on their overall accuracy compared to traditional 2D images.
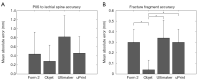
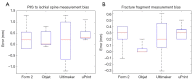
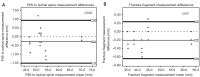
Results: Printing methodology did not affect the distance from PIIS to ischial spine (P=0.263). However, fracture fragment representation differed across 3D printed models, with the most accurate model produced by the high-end resin-based printer (P=0.007). The survey analysis showed that the low-cost printing methods produced models that were not as accurate in their representation of the fractured region (P=0.008).
Conclusions: The differences between models developed using traditional methods and low-cost methods have slight differences but may still provide useful information when developing a surgical plan.
Keywords: 3D printing; acetabular fracture; additive manufacturing; anatomic model; surgical planning.
2022 Annals of Translational Medicine. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://atm.amegroups.com/article/view/10.21037/atm-21-5069/coif). The authors have no conflicts of interest to declare.
Figures
References
Grants and funding
LinkOut - more resources
Full Text Sources
