The effect of screening on melanoma incidence and biopsy rates
- PMID: 35531668
- PMCID: PMC9796145
- DOI: 10.1111/bjd.21649
The effect of screening on melanoma incidence and biopsy rates
Abstract
Background: Cutaneous melanomas are common cancers in white-skinned populations, and early detection is promoted as a means of reducing morbidity and mortality. There is concern that increased skin screening is leading to overdiagnosis of indolent melanomas with low risk of lethality. The extent of melanoma overdiagnosis associated with screening is unknown.
Objectives: To estimate possible overdiagnosis by comparing subsequent melanoma incidence and biopsy rates among people subjected to skin screening those who were not.
Methods: We recruited 43 762 residents of Queensland, Australia, aged 40-69 years, with no prior history of melanoma, selected at random from a population register in 2010. At baseline, participants completed a comprehensive melanoma risk factor survey and were asked if their skin had been examined by a doctor in the 3 years prior to baseline. We calculated incidence and relative risk of histologically confirmed melanoma (invasive and in situ) in years 2-7 of follow-up, obtained through linkage to the cancer registry. In secondary analyses, we measured biopsy rates in years 2-6 of follow-up. We used propensity score analysis to calculate adjusted hazard ratios (aHRs) and 95% confidence intervals (CIs).
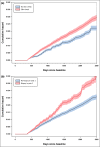
Results: In total, 28 155 participants underwent skin screening prior to baseline. We observed 967 first-incident melanomas (381 invasive) during 197 191 person-years of follow-up. Those screened had higher rates of melanoma (aHR 1·29, 95% CI 1·02-1·63) and subsequent skin biopses (aHR 1·85, 95% CI 1·69-2·04) than unscreened participants. The higher risk associated with skin screening was evident for in situ melanoma (aHR 1·45, 95% CI 1·09-1·92) but not invasive melanoma (aHR 1·05, 95% CI 0·72-1·54). In secondary analyses, where screening was defined as having a skin biopsy in the first year after baseline, we observed significantly increased risks of melanoma (aHR 1·53, 95% CI 1·23-1·89) and subsequent biopsies (aHR 2·64, 95% CI 2·46-2·84) relative to those who did not have a biopsy.
Conclusions: People who undergo skin screening subsequently experience higher rates of biopsies and melanoma (especially in situ melanoma), even after adjusting for all known risk factors, consistent with overdiagnosis. What is already known about this topic? Cutaneous melanomas are common cancers in white-skinned populations for which early detection is promoted as a means of reducing morbidity and mortality. There is concern that increased surveillance is leading to the overdiagnosis of indolent melanomas that are not destined to be lethal. The extent of melanoma overdiagnosis associated with surveillance is not known. What does this study add? People subjected to skin examinations by a doctor or who undergo skin biopsies subsequently have higher numbers of biopsies and higher rates of melanoma than people not subjected to either, even after adjusting for all known risk factors. These findings suggest that heightened surveillance leads to a proportion of melanomas being diagnosed that otherwise may not have come to clinical attention.
© 2022 The Authors. British Journal of Dermatology published by John Wiley & Sons Ltd on behalf of British Association of Dermatologists.
Conflict of interest statement
All authors have completed the ICMJE uniform disclosure form at
Figures
Comment in
-
Melanoma overdiagnosis: why it matters and what can be done about it.Br J Dermatol. 2022 Oct;187(4):459-460. doi: 10.1111/bjd.21750. Epub 2022 Aug 5. Br J Dermatol. 2022. PMID: 35929572 Free PMC article.
References
-
- Whiteman DC, Green AC, Olsen CM. The growing burden of invasive melanoma: projections of incidence rates and numbers of new cases in six susceptible populations through 2031. J Invest Dermatol 2016; 136:1161–71. - PubMed
-
- Adler NR, Kelly JW, Guitera P et al. Methods of melanoma detection and of skin monitoring for individuals at high risk of melanoma: new Australian clinical practice. Med J Aust 2019; 210:41–7. - PubMed
-
- Datzmann T, Schoffer O, Meier F et al. Patients benefit from participating in the German skin cancer screening program? A large cohort study based on administrative data. Br J Dermatol 2022; 186:69–77. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical