Spatial analysis of tuberculosis treatment outcomes in Shanghai: implications for tuberculosis control
- PMID: 35538695
- PMCID: PMC9684007
- DOI: 10.4178/epih.e2022045
Spatial analysis of tuberculosis treatment outcomes in Shanghai: implications for tuberculosis control
Abstract
Objectives: Tuberculosis (TB) treatment outcomes are a key indicator in the assessment of TB control programs. We aimed to identify spatial factors associated with TB treatment outcomes, and to provide additional insights into TB control from a geographical perspective.
Methods: We collected data from the electronic TB surveillance system in Shanghai, China and included pulmonary TB patients registered from January 1, 2009 to December 31, 2016. We examined the associations of physical accessibility to hospitals, an autoregression term, and random hospital effects with treatment outcomes in logistic regression models after adjusting for demographic, clinical, and treatment factors.
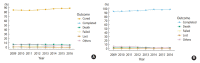
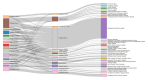
Results: Of the 53,475 pulmonary TB patients, 49,002 (91.6%) had successful treatment outcomes. The success rate increased from 89.3% in 2009 to 94.4% in 2016. The successful treatment outcome rate varied among hospitals from 78.6% to 97.8%, and there were 12 spatial clusters of poor treatment outcomes during the 8-year study period. The best-fit model incorporated spatial factors. Both the random hospital effects and autoregression terms had significant impacts on TB treatment outcomes, ranking 6th and 10th, respectively, in terms of statistical importance among 14 factors. The number of bus stations around the home was the least important variable in the model.
Conclusions: Spatial autocorrelation and hospital effects were associated with TB treatment outcomes in Shanghai. In highly-integrated cities like Shanghai, physical accessibility was not related to treatment outcomes. Governments need to pay more attention to the mobility of patients and different success rates of treatment among hospitals.
Keywords: China; Hospital effect; Physical accessibility; Spatial analysis; Treatment outcome; Tuberculosis.
Conflict of interest statement
The authors have no conflicts of interest to declare for this study.
Figures


Similar articles
-
Treatment outcomes and factors affecting treatment outcomes of new patients with tuberculosis in Busan, South Korea: a retrospective study of a citywide registry, 2014-2015.BMC Infect Dis. 2018 Dec 13;18(1):655. doi: 10.1186/s12879-018-3574-y. BMC Infect Dis. 2018. PMID: 30545315 Free PMC article.
-
Nutritional status and treatment outcomes of tuberculosis in Mizan Tepi University Teaching Hospital, a five -year retrospective study.PLoS One. 2024 Feb 15;19(2):e0298244. doi: 10.1371/journal.pone.0298244. eCollection 2024. PLoS One. 2024. PMID: 38359007 Free PMC article.
-
Socio-Demographic Predictors and Distribution of Pulmonary Tuberculosis (TB) in Xinjiang, China: A Spatial Analysis.PLoS One. 2015 Dec 7;10(12):e0144010. doi: 10.1371/journal.pone.0144010. eCollection 2015. PLoS One. 2015. PMID: 26641642 Free PMC article. Clinical Trial.
-
Treatment outcomes of childhood tuberculosis in Addis Ababa: a five-year retrospective analysis.BMC Public Health. 2016 Jul 21;16:612. doi: 10.1186/s12889-016-3193-8. BMC Public Health. 2016. PMID: 27443308 Free PMC article.
-
Which urban migrants default from tuberculosis treatment in Shanghai, China?PLoS One. 2013 Nov 28;8(11):e81351. doi: 10.1371/journal.pone.0081351. eCollection 2013. PLoS One. 2013. PMID: 24312292 Free PMC article.
Cited by
-
Tuberculosis treatment outcomes and associated factors among patients treated at Bosaso TB Hospital, Bosaso, Somalia: A five-year retrospective study.PLoS One. 2025 Jan 24;20(1):e0314693. doi: 10.1371/journal.pone.0314693. eCollection 2025. PLoS One. 2025. PMID: 39854532 Free PMC article.
-
Examining the efficacy of treatment outcomes for patients with pulmonary tuberculosis in Western China: A retrospective study in a region of high incidence.BMC Public Health. 2025 Apr 11;25(1):1360. doi: 10.1186/s12889-025-22543-4. BMC Public Health. 2025. PMID: 40217246 Free PMC article.
References
-
- World Health Organization Global tuberculosis report 2018. [cited 2021 Aug 26]. Available from: https://apps.who.int/iris/handle/10665/274453.
-
- Lawn SD, Zumla AI. Tuberculosis. Lancet. 2011;378:57–72. - PubMed
-
- Dye C, Watt CJ, Bleed DM, Hosseini SM, Raviglione MC. Evolution of tuberculosis control and prospects for reducing tuberculosis incidence, prevalence, and deaths globally. JAMA. 2005;293:2767–2775. - PubMed
-
- World Health Organization The global plan to stop TB, 2006-2015. 2016. [cited 2021 Aug 26]. Available from: https://apps.who.int/iris/handle/10665/43404. - PMC - PubMed

