Electronic Medical Record-Based Machine Learning Approach to Predict the Risk of 30-Day Adverse Cardiac Events After Invasive Coronary Treatment: Machine Learning Model Development and Validation
- PMID: 35544292
- PMCID: PMC9133980
- DOI: 10.2196/26801
Electronic Medical Record-Based Machine Learning Approach to Predict the Risk of 30-Day Adverse Cardiac Events After Invasive Coronary Treatment: Machine Learning Model Development and Validation
Abstract
Background: Although there is a growing interest in prediction models based on electronic medical records (EMRs) to identify patients at risk of adverse cardiac events following invasive coronary treatment, robust models fully utilizing EMR data are limited.
Objective: We aimed to develop and validate machine learning (ML) models by using diverse fields of EMR to predict the risk of 30-day adverse cardiac events after percutaneous intervention or bypass surgery.
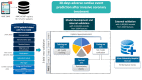
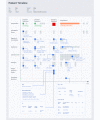
Methods: EMR data of 5,184,565 records of 16,793 patients at a quaternary hospital between 2006 and 2016 were categorized into static basic (eg, demographics), dynamic time-series (eg, laboratory values), and cardiac-specific data (eg, coronary angiography). The data were randomly split into training, tuning, and testing sets in a ratio of 3:1:1. Each model was evaluated with 5-fold cross-validation and with an external EMR-based cohort at a tertiary hospital. Logistic regression (LR), random forest (RF), gradient boosting machine (GBM), and feedforward neural network (FNN) algorithms were applied. The primary outcome was 30-day mortality following invasive treatment.
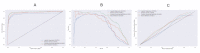
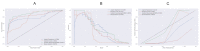
Results: GBM showed the best performance with area under the receiver operating characteristic curve (AUROC) of 0.99; RF had a similar AUROC of 0.98. AUROCs of FNN and LR were 0.96 and 0.93, respectively. GBM had the highest area under the precision-recall curve (AUPRC) of 0.80, and the AUPRCs of RF, LR, and FNN were 0.73, 0.68, and 0.63, respectively. All models showed low Brier scores of <0.1 as well as highly fitted calibration plots, indicating a good fit of the ML-based models. On external validation, the GBM model demonstrated maximal performance with an AUROC of 0.90, while FNN had an AUROC of 0.85. The AUROCs of LR and RF were slightly lower at 0.80 and 0.79, respectively. The AUPRCs of GBM, LR, and FNN were similar at 0.47, 0.43, and 0.41, respectively, while that of RF was lower at 0.33. Among the categories in the GBM model, time-series dynamic data demonstrated a high AUROC of >0.95, contributing majorly to the excellent results.
Conclusions: Exploiting the diverse fields of the EMR data set, the ML-based 30-day adverse cardiac event prediction models demonstrated outstanding results, and the applied framework could be generalized for various health care prediction models.
Keywords: adverse cardiac event; big data; coronary artery disease; electronic medical record; machine learning; mortality; prediction.
©Osung Kwon, Wonjun Na, Heejun Kang, Tae Joon Jun, Jihoon Kweon, Gyung-Min Park, YongHyun Cho, Cinyoung Hur, Jungwoo Chae, Do-Yoon Kang, Pil Hyung Lee, Jung-Min Ahn, Duk-Woo Park, Soo-Jin Kang, Seung-Whan Lee, Cheol Whan Lee, Seong-Wook Park, Seung-Jung Park, Dong Hyun Yang, Young-Hak Kim. Originally published in JMIR Medical Informatics (https://medinform.jmir.org), 11.05.2022.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures
Similar articles
-
Machine learning-based predictive models for perioperative major adverse cardiovascular events in patients with stable coronary artery disease undergoing noncardiac surgery.Comput Methods Programs Biomed. 2025 Mar;260:108561. doi: 10.1016/j.cmpb.2024.108561. Epub 2024 Dec 13. Comput Methods Programs Biomed. 2025. PMID: 39708562
-
Using machine learning methods to predict in-hospital mortality of sepsis patients in the ICU.BMC Med Inform Decis Mak. 2020 Oct 2;20(1):251. doi: 10.1186/s12911-020-01271-2. BMC Med Inform Decis Mak. 2020. PMID: 33008381 Free PMC article.
-
Development and validation of a prediction model for coronary heart disease risk in depressed patients aged 20 years and older using machine learning algorithms.Front Cardiovasc Med. 2025 Jan 9;11:1504957. doi: 10.3389/fcvm.2024.1504957. eCollection 2024. Front Cardiovasc Med. 2025. PMID: 39850379 Free PMC article.
-
Comparison of Multivariable Logistic Regression and Other Machine Learning Algorithms for Prognostic Prediction Studies in Pregnancy Care: Systematic Review and Meta-Analysis.JMIR Med Inform. 2020 Nov 17;8(11):e16503. doi: 10.2196/16503. JMIR Med Inform. 2020. PMID: 33200995 Free PMC article. Review.
-
Unveiling the utility of artificial intelligence for prediction, diagnosis, and progression of diabetic kidney disease: an evidence-based systematic review and meta-analysis.Curr Med Res Opin. 2024 Dec;40(12):2025-2055. doi: 10.1080/03007995.2024.2423737. Epub 2024 Nov 13. Curr Med Res Opin. 2024. PMID: 39474800
Cited by
-
Developing an Inpatient Electronic Medical Record Phenotype for Hospital-Acquired Pressure Injuries: Case Study Using Natural Language Processing Models.JMIR AI. 2023 Mar 8;2:e41264. doi: 10.2196/41264. JMIR AI. 2023. PMID: 38875552 Free PMC article.
-
Machine learning-based hybrid risk estimation system (ERES) in cardiac surgery: Supplementary insights from the ASA score analysis.PLOS Digit Health. 2025 Jun 23;4(6):e0000889. doi: 10.1371/journal.pdig.0000889. eCollection 2025 Jun. PLOS Digit Health. 2025. PMID: 40549810 Free PMC article.
-
A Machine Learning Approach to Differentiate Cold and Hot Syndrome in Viral Pneumonia Integrating Traditional Chinese Medicine and Modern Medicine: Machine Learning Model Development and Validation.JMIR Med Inform. 2025 Jul 16;13:e64725. doi: 10.2196/64725. JMIR Med Inform. 2025. PMID: 40669043 Free PMC article.
-
Leveraging BERT for embedding ICD codes from large scale cardiovascular EMR data to understand patient diagnostic patterns.BMC Med Inform Decis Mak. 2025 Aug 11;25(1):300. doi: 10.1186/s12911-025-03145-x. BMC Med Inform Decis Mak. 2025. PMID: 40790571 Free PMC article.
References
-
- Benjamin EJ, Muntner P, Alonso A, Bittencourt MS, Callaway CW, Carson AP, Chamberlain AM, Chang AR, Cheng S, Das SR, Delling FN, Djousse L, Elkind MSV, Ferguson JF, Fornage M, Jordan LC, Khan SS, Kissela BM, Knutson KL, Kwan TW, Lackland DT, Lewis TT, Lichtman JH, Longenecker CT, Loop MS, Lutsey PL, Martin SS, Matsushita K, Moran AE, Mussolino ME, O'Flaherty M, Pandey A, Perak AM, Rosamond WD, Roth GA, Sampson UKA, Satou GM, Schroeder EB, Shah SH, Spartano NL, Stokes A, Tirschwell DL, Tsao CW, Turakhia MP, VanWagner LB, Wilkins JT, Wong SS, Virani SS, American Heart Association Council on EpidemiologyPrevention Statistics CommitteeStroke Statistics Subcommittee Heart Disease and Stroke Statistics-2019 Update: A Report From the American Heart Association. Circulation. 2019 Mar 05;139(10):e56–e528. doi: 10.1161/CIR.0000000000000659. https://www.ahajournals.org/doi/abs/10.1161/CIR.0000000000000659?url_ver... - DOI - DOI - PubMed
-
- Neumann F, Sousa-Uva M, Ahlsson A, Alfonso F, Banning AP, Benedetto U, Byrne RA, Collet J, Falk V, Head SJ, Jüni P, Kastrati A, Koller A, Kristensen SD, Niebauer J, Richter DJ, Seferović PM, Sibbing D, Stefanini GG, Windecker S, Yadav R, Zembala MO. 2018 ESC/EACTS Guidelines on myocardial revascularization. EuroIntervention. 2019 Feb;14(14):1435–1534. doi: 10.4244/eijy19m01_01. - DOI - PubMed
-
- Weintraub WS, Grau-Sepulveda MV, Weiss JM, Delong ER, Peterson ED, O'Brien SM, Kolm P, Klein LW, Shaw RE, McKay C, Ritzenthaler LL, Popma JJ, Messenger JC, Shahian DM, Grover FL, Mayer JE, Garratt KN, Moussa ID, Edwards FH, Dangas GD. Prediction of long-term mortality after percutaneous coronary intervention in older adults: results from the National Cardiovascular Data Registry. Circulation. 2012 Mar 27;125(12):1501–10. doi: 10.1161/CIRCULATIONAHA.111.066969. http://europepmc.org/abstract/MED/22361329 CIRCULATIONAHA.111.066969 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources

