MRI tumour regression grade in locally recurrent rectal cancer
- PMID: 35552373
- PMCID: PMC9097816
- DOI: 10.1093/bjsopen/zrac033
MRI tumour regression grade in locally recurrent rectal cancer
Abstract
Background: This study aimed to investigate the agreement between magnetic resonance tumour regression grade (mrTRG) and pathological regression grade (pTRG) in patients with locally recurrent rectal cancer (LRRC). Also, the reproducibility of mrTRG was investigated.
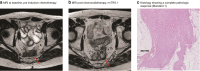
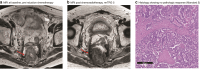
Methods: All patients with LRRC who underwent a resection between 2010 and 2018 after treatment with induction chemotherapy and neoadjuvant chemo(re)irradiation in whom a restaging MRI was available were retrospectively selected. All MRI scans were reassessed by two independent radiologists using the mrTRG, and the pTRG was reassessed by an independent pathologist. The interobserver agreement between the radiologists as well as between the radiologists and the pathologist was assessed with the weighted kappa test. A subanalysis was performed to evaluate the influence of the interval between imaging and surgery.
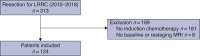
Results: Out of 313 patients with LRRC treated during the study interval, 124 patients were selected. Interobserver agreement between the radiologists was fair (k = 0.28) using a two-tier grading system (mrTRG 1-2 versus mrTRG 3-5). For the lead radiologist, agreement with pTRG was moderate (k = 0.52; 95 per cent c.i. 0.36 to 0.68) when comparing good (mrTRG 1-2 and Mandard 1-2) and intermediate/poor responders (mrTRG 3-5 and Mandard 3-5), and the agreement was fair between the other abdominal radiologist and pTRG (k = 0.39; 95 per cent c.i. 0.22 to 0.56). A shorter interval (less than 7 weeks) between MRI and surgery resulted in an improved agreement (k = 0.69), compared with an interval more than 7 weeks (k = 0.340). For the lead radiologist, the positive predictive value for predicting good responders was 95 per cent (95 per cent c.i. 71 per cent to 99 per cent), whereas this was 56 per cent (95 per cent c.i. 44 per cent to 66 per cent) for the other radiologist.
Conclusion: This study showed that, in LRRC, the reproducibility of mrTRG among radiologists is limited and the agreement of mrTRG with pTRG is low. However, a shorter interval between MRI and surgery seems to improve this agreement and, if assessed by a dedicated radiologist, mrTRG could predict good responders.
© The Author(s) 2022. Published by Oxford University Press on behalf of BJS Society Ltd.
Figures



References
-
- Siddiqui MRS, Gormly KL, Bhoday J, Balyansikova S, Battersby NJ, Chand Met al. Interobserver agreement of radiologists assessing the response of rectal cancers to preoperative chemoradiation using the MRI tumour regression grading (mrTRG). Clin Radiol 2016;71:854–862 - PubMed
-
- Patel UB, Taylor F, Blomqvist L, George C, Evans H, Tekkis Pet al. Magnetic resonance imaging-detected tumor response for locally advanced rectal cancer predicts survival outcomes: MERCURY experience. J Clin Oncol 2011;29:3753–3760 - PubMed
-
- Bosman SJ, Holman FA, Nieuwenhuijzen GAP, Martijn H, Creemers GJ, Rutten HJT. Feasibility of reirradiation in the treatment of locally recurrent rectal cancer. Br J Surg 2014;101:1280–1289 - PubMed
-
- van der Meij W, Rombouts AJM, Rutten H, Bremers AJA, De Wilt JHW. Treatment of locally recurrent rectal carcinoma in previously (chemo)irradiated patients: a review. Dis Colon Rectum 2016;59:148–156 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

