Comparison of the effects of perineural or intravenous dexamethasone on thoracic paravertebral block in Ivor-Lewis esophagectomy: A double-blind randomized trial
- PMID: 35570329
- PMCID: PMC9372414
- DOI: 10.1111/cts.13304
Comparison of the effects of perineural or intravenous dexamethasone on thoracic paravertebral block in Ivor-Lewis esophagectomy: A double-blind randomized trial
Abstract
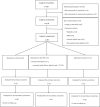
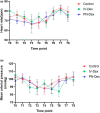
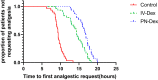
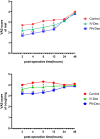
Efforts to prolong thoracic paravertebral block (TPVB) analgesia include local anesthetic adjuvants, such as dexamethasone (Dex). Previous studies showed that both perineural (PN) and intravenous (i.v.) routes could prolong analgesia. As PN Dex is an off-label use, anesthesiologists should be fully informed of the clinical differences, if any, on block duration. This study was designed to evaluate the two administration routes of Dex for duration of analgesia in TPVB. Ninety-five patients scheduled for Ivor-Lewis esophagectomy were randomized to receive TPVB (0.5% ropivacaine 15 ml), PN or i.v. Dex 8 mg. The primary end point was the duration of analgesia. The secondary end points included pain scores, analgesic consumption, adverse effects rate, and incidence of chronic pain at 3 months postoperatively. The PN-Dex group showed better analgesic effects than the i.v.-Dex group (p < 0.05). Similarly, the visual analogue scale scores in patients at 2, 4, 8, and 12 h postoperatively were lower in the PN-Dex group than the i.v.-Dex group (p < 0.05). The analgesic consumption in both the PN-Dex and i.v.-Dex groups was significantly lower than that in the control group (p < 0.05). Regarding the incidence of chronic pain, regardless of route, Dex decreased the incidence of chronic postsurgical pain and neuropathic pain at 3 months after surgery (p < 0.05), but there were no clinical differences between the i.v.-Dex and PN-Dex groups. Perineural dexamethasone improved the magnitude and duration of analgesia compared to that of the i.v.-Dex group in TPVB in Ivor-Lewis esophagectomy. However, there were no clinically significant differences between the two groups in the incidence of chronic pain.
© 2022 The Authors. Clinical and Translational Science published by Wiley Periodicals LLC on behalf of American Society for Clinical Pharmacology and Therapeutics.
Conflict of interest statement
The authors declared no competing interests for this work.
Figures
References
-
- Brown MJ, Kor DJ, Allen MS, et al. Dual‐epidural catheter technique and perioperative outcomes after Ivor‐Lewis esophagectomy. Reg Anesth Pain Med. 2013;38(1):3‐8. - PubMed
-
- Booka E, Nakano Y, Mihara K, et al. The impact of epidural catheter insertion level on pain control after esophagectomy for esophageal cancer. Esophagus. 2020;17(2):175‐182. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

