Cardiovascular Benefit of Continuous Positive Airway Pressure in Adults with Coronary Artery Disease and Obstructive Sleep Apnea without Excessive Sleepiness
- PMID: 35579605
- PMCID: PMC9799106
- DOI: 10.1164/rccm.202111-2608OC
Cardiovascular Benefit of Continuous Positive Airway Pressure in Adults with Coronary Artery Disease and Obstructive Sleep Apnea without Excessive Sleepiness
Abstract
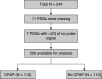
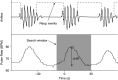
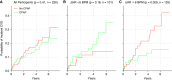
Rationale: Randomized controlled trials of continuous positive airway pressure (CPAP) in patients with obstructive sleep apnea (OSA) have not demonstrated protection against adverse cardiovascular outcomes. Recently, observational studies revealed that OSA-related cardiovascular risk is concentrated in patients with an elevated pulse rate response to respiratory events (ΔHR). Objectives: Here, in this post hoc analysis of a prospective clinical trial, we test the hypothesis that a greater pretreatment ΔHR is associated with greater CPAP-related protection against adverse cardiovascular outcomes. Methods: ΔHR was measured from baseline polysomnography of the RICCADSA (Randomized Intervention with CPAP in CAD and OSA) randomized controlled trial (patients with coronary artery disease [CAD] and OSA [apnea-hypopnea index ⩾ 15 events/h] with Epworth Sleepiness Scale score < 10; nCPAP:ncontrol = 113:113; male, 85%; age, 66 ± 8 [mean ± SD] yr). The primary outcome was a composite of repeat revascularization, myocardial infarction, stroke, and cardiovascular mortality. Multivariable Cox regression assessed whether the effect of CPAP was moderated by ΔHR (treatment-by-ΔHR interaction). Measurements and Main Results: The CPAP-related reduction in risk increased progressively with increasing pretreatment ΔHR (interaction hazard ratio [95% confidence interval], 0.49 [0.27 to 0.90] per SD increase in ΔHR; P < 0.05). This means that in patients with a ΔHR of 1 SD above the mean (i.e., 10 beats/min), CPAP was estimated to reduce cardiovascular risk by 59% (6% to 82%) (P < 0.05), but no significant risk reduction was estimated in patients with a mean ΔHR (6 beats/min; CPAP risk reduction, 16% [-53% to 54%]; P = 0.6). Conclusions: The protective effect of CPAP in patients with CAD and OSA without excessive sleepiness was modified by the ΔHR. Specifically, patients with higher ΔHR exhibit greater cardiovascular benefit from CPAP therapy.
Keywords: cardiovascular; clinical trial; heart rate response; sleep apnea; sleepiness.
Figures
Comment in
-
Continuous Positive Airway Pressure and Cardiovascular Risk Reduction in Patients without Excessive Sleepiness: Importance of the Pulse Rate Response.Am J Respir Crit Care Med. 2022 Sep 15;206(6):666-667. doi: 10.1164/rccm.202206-1050ED. Am J Respir Crit Care Med. 2022. PMID: 35675563 Free PMC article. No abstract available.
-
Heart Rate Response in OSA: A Clue to Reveal Cardiovascular Benefit from CPAP?Am J Respir Crit Care Med. 2022 Nov 1;206(9):1180-1181. doi: 10.1164/rccm.202205-0984LE. Am J Respir Crit Care Med. 2022. PMID: 35863079 Free PMC article. No abstract available.
-
Reply to: Heart Rate Response in Obstructive Sleep Apnea: A Clue to Reveal Cardiovascular Benefit from Continuous Positive Airway Pressure?Am J Respir Crit Care Med. 2022 Nov 1;206(9):1181-1182. doi: 10.1164/rccm.202207-1348LE. Am J Respir Crit Care Med. 2022. PMID: 35863081 Free PMC article. No abstract available.
References
-
- Veasey SC, Rosen IM. Obstructive sleep apnea in adults. N Engl J Med . 2019;380:1442–1449. - PubMed
-
- Campos-Rodriguez F, Martinez-Garcia MA, de la Cruz-Moron I, Almeida-Gonzalez C, Catalan-Serra P, Montserrat JM. Cardiovascular mortality in women with obstructive sleep apnea with or without continuous positive airway pressure treatment: a cohort study. Ann Intern Med . 2012;156:115–122. - PubMed
Publication types
MeSH terms
Grants and funding
- R21 HL167126/HL/NHLBI NIH HHS/United States
- UL1 TR001863/TR/NCATS NIH HHS/United States
- R01 HL102321/HL/NHLBI NIH HHS/United States
- R01HL153874/GF/NIH HHS/United States
- R35 HL135818/HL/NHLBI NIH HHS/United States
- K23 HL159259/HL/NHLBI NIH HHS/United States
- R01 HL128658/HL/NHLBI NIH HHS/United States
- R21 HL161766/HL/NHLBI NIH HHS/United States
- R01 HL153874/HL/NHLBI NIH HHS/United States
- UL1 RR025758/RR/NCRR NIH HHS/United States
- R01 HL146697/HL/NHLBI NIH HHS/United States
- P01 HL095491/HL/NHLBI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

