Acute respiratory distress syndrome after in-hospital cardiac arrest
- PMID: 35580706
- PMCID: PMC9320405
- DOI: 10.1016/j.resuscitation.2022.05.006
Acute respiratory distress syndrome after in-hospital cardiac arrest
Abstract
Objective: Acute respiratory distress syndrome (ARDS) after out-of-hospital cardiac arrest is common and associated with worse outcomes. In the hospital setting, there are many potential risk factors for post-arrest ARDS, such as aspiration, sepsis, and shock. ARDS after in-hospital cardiac arrest (IHCA) has not been characterized.
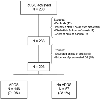
Methods: We performed a single-center retrospective study of adult patients admitted to the hospital between 2014-2018 who suffered an IHCA, achieved return of spontaneous circulation (ROSC), and were either already intubated at the time of arrest or within 2 hours of ROSC. Post-IHCA ARDS was defined as meeting the Berlin criteria in the first 3 days following ROSC. Outcomes included alive-and-ventilator free days across 28 days, hospital length-of-stay, hospital mortality, and hospital disposition.
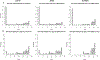
Results: Of 203 patients included, 146 (71.9%) developed ARDS. In unadjusted analysis, patients with ARDS had fewer alive-and-ventilator-free days over 28 days with a median of 1 (IQR: 0, 21) day, compared to 18 (IQR: 0, 25) days in patients without ARDS (p = 0.03). However, this association was not significant after multivariate adjustment. There was also a non-significant longer hospital length-of-stay (15 [IQR: 7, 26] vs 10 [IQR: 7, 22] days, p = 0.25; median adjusted increase in ARDS patients: 3 [95% CI: -2 to 8] days, p = 0.27) and higher hospital mortality (53% vs 44%, p = 0.26; aOR 1.6 [95% CI: 0.8-2.9], p = 0.17) in the ARDS group.
Conclusion: Among IHCA patients, almost three-quarters developed ARDS within 3 days of ROSC. As in out of hospital cardiac arrest, post-IHCA ARDS is common.
Keywords: ARDS; Cardiac arrest; Resuscitation.
Copyright © 2022 Elsevier B.V. All rights reserved.
Conflict of interest statement
Conflict of Interest
The manuscript has not been published previously and is not under consideration in another journal. The authors report no external funding source for this study and declare no conflict of interest.
Figures
Comment in
-
Don't go breaking my…lungs? The acute respiratory distress syndrome is common, deadly, and probably underrecognized after cardiac arrest.Resuscitation. 2022 Aug;177:1-2. doi: 10.1016/j.resuscitation.2022.06.002. Epub 2022 Jun 10. Resuscitation. 2022. PMID: 35697174 Free PMC article. No abstract available.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials