Insomnia disorders are associated with increased cardiometabolic disturbances and death risks from cardiovascular diseases in psychiatric patients treated with weight-gain-inducing psychotropic drugs: results from a Swiss cohort
- PMID: 35581641
- PMCID: PMC9116036
- DOI: 10.1186/s12888-022-03983-3
Insomnia disorders are associated with increased cardiometabolic disturbances and death risks from cardiovascular diseases in psychiatric patients treated with weight-gain-inducing psychotropic drugs: results from a Swiss cohort
Erratum in
-
Publisher Correction: Insomnia disorders are associated with increased cardiometabolic disturbances and death risks from cardiovascular diseases in psychiatric patients treated with weight-gain-inducing psychotropic drugs: results from a Swiss cohort.BMC Psychiatry. 2022 Jul 8;22(1):457. doi: 10.1186/s12888-022-04040-9. BMC Psychiatry. 2022. PMID: 35804331 Free PMC article. No abstract available.
Abstract
Study objectives: Insomnia disorders as well as cardiometabolic disorders are highly prevalent in the psychiatric population compared to the general population. We aimed to investigate their association and evolution over time in a Swiss psychiatric cohort.
Methods: Data for 2861 patients (8954 observations) were obtained from two prospective cohorts (PsyMetab and PsyClin) with metabolic parameters monitored routinely during psychotropic treatment. Insomnia disorders were based on the presence of ICD-10 "F51.0" diagnosis (non-organic insomnia), the prescription of sedatives before bedtime or the discharge letter. Metabolic syndrome was defined using the International Diabetes Federation definition, while the 10-year risk of cardiovascular event or death was assessed using the Framingham Risk Score and the Systematic Coronary Risk Estimation, respectively.
Results: Insomnia disorders were observed in 30% of the cohort, who were older, predominantly female, used more psychotropic drugs carrying risk of high weight gain (olanzapine, clozapine, valproate) and were more prone to suffer from schizoaffective or bipolar disorders. Multivariate analyses showed that patients with high body mass index (OR = 2.02, 95%CI [1.51-2.72] for each ten-kg/m2 increase), central obesity (OR = 2.20, [1.63-2.96]), hypertension (OR = 1.86, [1.23-2.81]), hyperglycemia (OR = 3.70, [2.16-6.33]), high density lipoprotein hypocholesterolemia in women (OR = 1.51, [1.17-1.95]), metabolic syndrome (OR = 1.84, [1.16-2.92]) and higher 10-year risk of death from cardiovascular diseases (OR = 1.34, [1.17-1.53]) were more likely to have insomnia disorders. Time and insomnia disorders were associated with a deterioration of cardiometabolic parameters.
Conclusions: Insomnia disorders are significantly associated with metabolic worsening and risk of death from cardiovascular diseases in psychiatric patients.
Keywords: Cardiovascular diseases; Insomnia disorders; Metabolic syndrome; Metabolic worsening; Psychiatry.
© 2022. The Author(s).
Conflict of interest statement
CBE received honoraria for conferences from Forum pour la formation médicale, Janssen-Cilag, Lundbeck, Otsuka, Sandoz, Servier, Sunovion, Sysmex Suisse AG, Takeda, Vifor-Pharma, and Zeller in the past 3 years. NA received honoraria for a conference from Sysmex Suisse AG in the past 3 years. FV received honoraria for conferences or teaching CME courses from Forum für Medizinische Fortbildung and Sysmex Suisse AG in the past 3 years. HRL received honoraria for conferences from Sandoz and Sunovion in the past 3 years. SC received honoraria for conferences from Forum pour la formation médicale in the past 3 years. All the other authors declare that they have no conflict of interest in relation to the content of this paper.
Figures

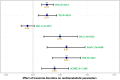
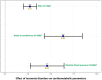
Similar articles
-
Evaluation of Cardiometabolic Risk in a Large Psychiatric Cohort and Comparison With a Population-Based Sample in Switzerland.J Clin Psychiatry. 2020 Mar 31;81(3):19m12796. doi: 10.4088/JCP.19m12796. J Clin Psychiatry. 2020. PMID: 32237298
-
Prevalence of obesity, metabolic syndrome, diabetes and risk of cardiovascular disease in a psychiatric inpatient sample: results of the Metabolism in Psychiatry (MiP) Study.Eur Arch Psychiatry Clin Neurosci. 2020 Aug;270(5):597-609. doi: 10.1007/s00406-019-01043-8. Epub 2019 Jul 13. Eur Arch Psychiatry Clin Neurosci. 2020. PMID: 31302731
-
Socio-economic position as a moderator of cardiometabolic outcomes in patients receiving psychotropic treatment associated with weight gain: results from a prospective 12-month inception cohort study and a large population-based cohort.Transl Psychiatry. 2021 Jun 26;11(1):360. doi: 10.1038/s41398-021-01482-9. Transl Psychiatry. 2021. PMID: 34226496 Free PMC article.
-
[Psychotropic drugs induced weight gain: a review of the literature concerning epidemiological data, mechanisms and management].Encephale. 2005 Jul-Aug;31(4 Pt 1):507-16. doi: 10.1016/s0013-7006(05)82412-1. Encephale. 2005. PMID: 16389718 Review. French.
-
Cardiometabolic effects of psychotropic medications.Horm Mol Biol Clin Investig. 2018 Jan 10;36(1):/j/hmbci.2018.36.issue-1/hmbci-2017-0065/hmbci-2017-0065.xml. doi: 10.1515/hmbci-2017-0065. Horm Mol Biol Clin Investig. 2018. PMID: 29320364 Free PMC article. Review.
Cited by
-
Incidence of adverse cardiovascular events in patients with insomnia: A systematic review and meta-analysis of real-world data.PLoS One. 2023 Sep 21;18(9):e0291859. doi: 10.1371/journal.pone.0291859. eCollection 2023. PLoS One. 2023. PMID: 37733726 Free PMC article.
-
Metabolic Adverse Effects of Psychotropic Drug Therapy: A Systematic Review.Eur J Investig Health Psychol Educ. 2023 Aug 12;13(8):1505-1520. doi: 10.3390/ejihpe13080110. Eur J Investig Health Psychol Educ. 2023. PMID: 37623307 Free PMC article. Review.
-
Effects of electrostatic therapy on nighttime sleep and daytime symptoms in patients with chronic insomnia: Evidences from an open label study.Front Neurosci. 2023 Jan 6;16:1047240. doi: 10.3389/fnins.2022.1047240. eCollection 2022. Front Neurosci. 2023. PMID: 36685220 Free PMC article.
-
Metabolic syndrome and its components are associated with lengths of stay in a psychiatric hospital: Results from a Swiss psychiatric cohort and first-episode psychosis patients.Eur Psychiatry. 2025 May 26;68(1):e65. doi: 10.1192/j.eurpsy.2025.10036. Eur Psychiatry. 2025. PMID: 40415581 Free PMC article.
-
Insomnia, Short Sleep, and Their Treatments: Review of Their Associations with Weight.Curr Obes Rep. 2024 Jun;13(2):203-213. doi: 10.1007/s13679-024-00570-3. Epub 2024 May 22. Curr Obes Rep. 2024. PMID: 38776004 Free PMC article. Review.
References
-
- C. Dubath et al. Evaluation of Cardiometabolic Risk in a Large Psychiatric Cohort and Comparison With a Population-Based Sample in Switzerland, J. Clin. Psychiatry. 2020; 81:3. 10.4088/JCP.19m12796. - PubMed
-
- T. Ma, T. Mackinnon, et K. Dean. The prevalence of cardiometabolic disease in people with psychotic disorders in secure settings – a systematic review. J. Forensic Psychiatry Psychol. 2020; 0, no 0:1‑27. 10.1080/14789949.2020.1859588.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

