Perinatal mortality and its predictors in Kersa Health and Demographic Surveillance System, Eastern Ethiopia: population-based prospective study from 2015 to 2020
- PMID: 35584868
- PMCID: PMC9119174
- DOI: 10.1136/bmjopen-2021-054975
Perinatal mortality and its predictors in Kersa Health and Demographic Surveillance System, Eastern Ethiopia: population-based prospective study from 2015 to 2020
Abstract
Objective: Perinatal mortality is an important outcome indicator for newborn care and directly mirrors the quality of prenatal, intra partum and newborn care. Therefore, this study was aimed at estimating perinatal mortality and its predictors in Eastern Ethiopia using data from Kersa Health and Demographic Surveillance System (KHDSS).
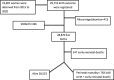
Design, settings and participants: An open dynamic cohort design was employed among pregnant women from 2015 to 2020 at KHDSS. A total of 19 687 women were observed over the period of 6 years, and 29 719 birth outcomes were registered.
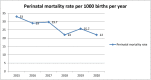
Outcome measures: Perinatal mortality rate was estimated for each year of cohort and the cumulative of 6 years. Predictors of perinatal mortality are identified.
Results: From a total of 29 306 births 783 (26.72 deaths per 1000 births; 95% CI 24.88 to 28.66) deaths were occurred during perinatal period. Rural residence (adjusted OR (AOR)=3.43; 95% CI 2.04 to 5.76), birth weight (low birth weight, AOR=3.98; 95% CI 3.04 to 5.20; big birth weight, AOR=2.51; 95% CI 1.76 to 3.57), not having antenatal care (ANC) (AOR=1.67; 95% CI 1.29 to 2.17) were associated with higher odds of perinatal mortality whereas the parity (multipara, AOR=0.46; 95% CI 0.34 to 0.62; grand multipara, AOR=0.31; 95% CI 0.21 to 0.47) was associated with lower odds of perinatal mortality.
Conclusions: The study revealed relatively high perinatal mortality rate. Place of residence, ANC, parity and birth weight were identified as predictors of perinatal mortality. Devising strategies that enhance access to and utilisations of ANC services with due emphasis for rural residents, primipara mothers and newborn with low and big birth weights may be crucial for reducing perinatal mortality.
Keywords: EPIDEMIOLOGY; Fetal medicine; PERINATOLOGY.
© Author(s) (or their employer(s)) 2022. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures
Similar articles
-
Trends in congenital anomalies and associated factors among newborns in Eastern Ethiopia: an 8-year open cohort analysis of the Kersa Health and Demographic Surveillance System.BMJ Open. 2025 Feb 3;15(2):e089984. doi: 10.1136/bmjopen-2024-089984. BMJ Open. 2025. PMID: 39900415 Free PMC article.
-
Predictors of perinatal mortality in rural population of Northwest Ethiopia: a prospective longitudinal study.BMC Public Health. 2013 Feb 23;13:168. doi: 10.1186/1471-2458-13-168. BMC Public Health. 2013. PMID: 23433304 Free PMC article.
-
Determinants of perinatal mortality among cohorts of pregnant women in three districts of North Showa zone, Oromia Region, Ethiopia: Community based nested case control study.BMC Public Health. 2018 Jul 18;18(1):888. doi: 10.1186/s12889-018-5757-2. BMC Public Health. 2018. PMID: 30021557 Free PMC article.
-
Individual and community-level factors of perinatal mortality in the high mortality regions of Ethiopia: a multilevel mixed-effect analysis.BMC Public Health. 2022 Feb 7;22(1):247. doi: 10.1186/s12889-022-12695-y. BMC Public Health. 2022. PMID: 35130852 Free PMC article.
-
Perinatal mortality and its association with antenatal care visit, maternal tetanus toxoid immunization and partograph utilization in Ethiopia: a meta-analysis.Sci Rep. 2021 Oct 4;11(1):19641. doi: 10.1038/s41598-021-98996-5. Sci Rep. 2021. PMID: 34608180 Free PMC article.
Cited by
-
Predictors of perinatal mortality in Liberia's post-civil unrest: A comparative analysis of the 2013 and 2019-2020 Liberia Demographic and Health Surveys.BMJ Open. 2024 Feb 27;14(2):e080661. doi: 10.1136/bmjopen-2023-080661. BMJ Open. 2024. PMID: 38417962 Free PMC article.
-
Perinatal mortality and its predictors in Beni City, Democratic Republic of Congo: a cross-sectional study.Matern Health Neonatol Perinatol. 2024 Jul 5;10(1):14. doi: 10.1186/s40748-024-00184-6. Matern Health Neonatol Perinatol. 2024. PMID: 38965609 Free PMC article.
-
Pooled estimates of stillbirth in Ethiopia: systematic review and meta-analysis, 2013-2024.J Health Popul Nutr. 2025 Apr 19;44(1):126. doi: 10.1186/s41043-025-00877-4. J Health Popul Nutr. 2025. PMID: 40253383 Free PMC article.
-
Why Babies die in the first 7 days after birth in Somalia Region of Ethiopia?Ann Med Surg (Lond). 2023 Apr 18;85(5):1821-1825. doi: 10.1097/MS9.0000000000000690. eCollection 2023 May. Ann Med Surg (Lond). 2023. PMID: 37228995 Free PMC article.
-
Analysis of regional heterogeneity and determinants of perinatal mortality in Ethiopia: review.Ann Med Surg (Lond). 2023 Mar 27;85(4):902-907. doi: 10.1097/MS9.0000000000000400. eCollection 2023 Apr. Ann Med Surg (Lond). 2023. PMID: 37113814 Free PMC article.
References
-
- Bakketeig LS, Bergsjø P, Epidemiology P. International encyclopedia of public health. Oxford: Academic Press, 2008: 45–53.
-
- EMI SUZUKI HK . A neglected burden: the global tragedy of stillbirths stillbirths: report of the un Inter-Agency group for child mortality estimation, 2020. Available: https://blogs.worldbank.org/opendata/first-ever-un-report-global-stillbi...
-
- Wang H, Bhutta ZA, Coates MM, et al. . Global, regional, National, and selected subnational levels of stillbirths, neonatal, infant, and under-5 mortality, 1980-2015: a systematic analysis for the global burden of disease study 2015. Lancet 2016;388:1725–74. 10.1016/S0140-6736(16)31575-6 - DOI - PMC - PubMed
-
- Estimation UNIGfCM . Levels & Trends in Child Mortality: Report 2017: Estimates Developed by the UN Inter-Agency Group for Child Mortality Estimation. United Nations Children’s Fund, 2017.
MeSH terms
LinkOut - more resources
Full Text Sources