Poor prognosis of patients with severe COVID-19 admitted to an infectious disease intensive care unit during the pandemic caused by the Delta variant in Japan
- PMID: 35586761
- PMCID: PMC9066459
- DOI: 10.35772/ghm.2021.01121
Poor prognosis of patients with severe COVID-19 admitted to an infectious disease intensive care unit during the pandemic caused by the Delta variant in Japan
Abstract
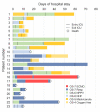
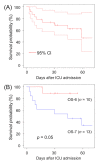
During the surge of coronavirus disease (COVID-19) caused by the severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) delta variant, our institution operated an intensive care unit (ICU) for patients with severe COVID-19. The study aim was to determine the survival rate and treatment outcomes of patients with severe COVID-19 treated in the ICU during the surge. A total of 23 consecutive patients with severe COVID-19 were admitted to the ICU between August 5 and October 6, 2021. Patients received multidrug therapy consisting of remdesivir, tocilizumab, heparin, and methylprednisolone. The patients were divided into two groups based on the ordinal scale (OS): a non-invasive oxygen therapy (OS-6) group, and an invasive oxygen therapy (OS-7) group. There were 13 (57%) and 10 (43%) patients in the OS-7 and OS-6 groups, respectively. All patients were unvaccinated. Sixteen patients (70%) were male. The median age was 53 years; the median body mass index (BMI) was 30.3 kg/m2; and the median P/F ratio on admission was 96. The 30-day survival rate was 69% and was significantly poorer in the OS-7 group (54%) than in the OS-6 group (89%; p = 0.05). The prevalence of obesity (p = 0.05) and the Sequential Organ Failure Assessment (SOFA) score on admission (p < 0.01) were significantly higher in the OS-7 group. Seven patients in the OS-7 group (54%) developed bacteremia. A low P/F ratio on admission was a significant unfavorable prognostic factor (hazard ratio: 10.9; p = 0.03). The survival rate was poor, especially in patients requiring invasive oxygen therapy. More measures are needed to improve the treatment outcomes of patients with severe COVID 19.
Keywords: SARS-CoV-2 infection; mechanical ventilation; mortality; secondary hospital-acquired infection.
2022, National Center for Global Health and Medicine.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures
Similar articles
-
Safety and Efficacy of Imatinib for Hospitalized Adults with COVID-19: A structured summary of a study protocol for a randomised controlled trial.Trials. 2020 Oct 28;21(1):897. doi: 10.1186/s13063-020-04819-9. Trials. 2020. PMID: 33115543 Free PMC article.
-
Double-blind, randomized, controlled, trial to assess the efficacy of allogenic mesenchymal stromal cells in patients with acute respiratory distress syndrome due to COVID-19 (COVID-AT): A structured summary of a study protocol for a randomised controlled trial.Trials. 2021 Jan 6;22(1):9. doi: 10.1186/s13063-020-04964-1. Trials. 2021. PMID: 33407777 Free PMC article.
-
Covid-19 severe hypoxemic pneumonia: A clinical experience using high-flow nasal oxygen therapy as first-line management.Respir Med Res. 2021 Nov;80:100834. doi: 10.1016/j.resmer.2021.100834. Epub 2021 Jun 4. Respir Med Res. 2021. PMID: 34153702 Free PMC article.
-
Outcomes of patients with COVID-19 acute respiratory distress syndrome requiring invasive mechanical ventilation admitted to an intensive care unit in South Africa.S Afr Med J. 2022 Feb 2;112(1):13516. S Afr Med J. 2022. PMID: 35140002
-
Intensive care management of patients with COVID-19: a practical approach.Ann Intensive Care. 2021 Feb 18;11(1):36. doi: 10.1186/s13613-021-00820-w. Ann Intensive Care. 2021. PMID: 33604873 Free PMC article. Review.
Cited by
-
Predictors of negative outcomes in hospitalized patients with SARS‑CoV‑2 pneumonia: A retrospective study.Exp Ther Med. 2023 Jul 31;26(3):437. doi: 10.3892/etm.2023.12137. eCollection 2023 Sep. Exp Ther Med. 2023. PMID: 37614431 Free PMC article.
-
Vaccination Status and Number of Vaccine Doses Are Independently Associated with the PaO2/FiO2 Ratio on Admission in Hospitalized COVID-19 Patients.Vaccines (Basel). 2022 Aug 29;10(9):1424. doi: 10.3390/vaccines10091424. Vaccines (Basel). 2022. PMID: 36146502 Free PMC article.
-
Factors associated with the outcome of patients with COVID-19 requiring mechanical ventilation: A single-center observational study in Japan.Acute Med Surg. 2023 Jul 8;10(1):e868. doi: 10.1002/ams2.868. eCollection 2023 Jan-Dec. Acute Med Surg. 2023. PMID: 37424772 Free PMC article.
-
A cost-effectiveness analysis of COVID-19 critical care interventions in Addis Ababa, Ethiopia: a modeling study.Cost Eff Resour Alloc. 2023 Jun 26;21(1):40. doi: 10.1186/s12962-023-00446-8. Cost Eff Resour Alloc. 2023. PMID: 37365623 Free PMC article.
References
-
- Japanese Ministry of Health, Labour and Welfare. COVID-19 in Japan. https://www.mhlw.go.jp/stf/covid-19/kokunainohasseijoukyou.html (accessed November 16, 2021). (in Japanese) .
LinkOut - more resources
Full Text Sources
Miscellaneous

