Ocular mycobacterial lesions in cats
- PMID: 35587045
- PMCID: PMC9358306
- DOI: 10.1177/03009858221098431
Ocular mycobacterial lesions in cats
Abstract
Ocular mycobacterial infections are an under-recognized cause of morbidity in the domestic cat. This study aimed to explore the distribution, histopathological appearance, and severity of feline ocular mycobacterial lesions, and to characterize the immune cell population with immunohistochemistry. Routine histological staining with hematoxylin and eosin, and Masson's trichrome, was performed to identify ocular lesions and assign an inflammation score based on the number of cells present. Acid-fast bacilli were detected with Ziehl-Neelsen, and immunohistochemistry for ionized calcium-binding adaptor protein-1 (Iba1), calprotectin, cluster of differentiation 3 (CD3), and Pax5 was undertaken on formalin-fixed paraffin-embedded tissue samples from 24 cases of ocular mycobacteriosis. Posterior or panuveitis with concurrent retinitis was identified in 20/24 cases (83%), with retinal detachment in 16/20 (80%) of these cases. Choroidal lesions had the highest median inflammation score. Ziehl-Neelsen-positive organisms were detected in 20/24 cases (83%), with the highest prevalence of acid-fast bacilli detected in choroidal lesions (16/20, 80%). Lesions were typically granulomatous to pyogranulomatous, characterized by abundant numbers of Iba1-positive macrophages, followed by calprotectin-positive granulocytes and monocytes, fewer T cells, and rarer B cells. However, where iritis was identified, inflammation was typically lymphoplasmacytic (11/16 cases, 69%). Where diagnostic testing was performed, tuberculosis (ie, infection with Mycobacterium bovis, Mycobacterium microti, or a nonspeciated Mycobacterium tuberculosis-complex pathogen) was diagnosed in 20/22 cats (91%), with Mycobacterium lepraemurium infection identified in the other 2/22 cats (9%). These results suggest the choroid is the primary site of lesion development in most cases of feline ocular mycobacteriosis, and inflammatory changes are associated with the presence of mycobacteria localized to ocular tissues.
Keywords: cats; eye; histopathology; immunohistochemistry; mycobacteria; tuberculosis.
Conflict of interest statement
Figures

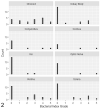


References
-
- Agarwal A, Agrawal R, Gunasekaran DV, et al. The Collaborative Ocular Tuberculosis Study (COTS)-1 Report 3: polymerase chain reaction in the diagnosis and management of tubercular uveitis: global trends. Ocul Immunol Inflamm. 2019;27:465–473. - PubMed
-
- Agostinelli C, Sabattini E, Gjørret JO, et al. Characterization of a new monoclonal antibody against Pax5/BASP in 1525 paraffin-embedded human and animal tissue samples. Appl Immunohistochem Mol Morphol. 2010;18:561–572. - PubMed
-
- Aguilar JP, Green WR. Choroidal rupture. A histopathologic study of 47 cases. Retina. 1984;4:269–275. - PubMed
-
- Anderson DH, Stern WH, Fisher SK, et al. Retinal detachment in the cat: the pigment epithelial-photoreceptor interface. Invest Ophthalmol Vis Sci. 1983;24:906–926. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

