Emergency and post-emergency care of older adults with Alzheimer's disease/Alzheimer's disease related dementias
- PMID: 35612546
- PMCID: PMC9489611
- DOI: 10.1111/jgs.17833
Emergency and post-emergency care of older adults with Alzheimer's disease/Alzheimer's disease related dementias
Abstract
Background: The emergency department (ED) is a critical juncture in the care of persons living with dementia (PLwD), as they have a high rate of hospital admission, ED revisits, and subsequent inpatient stays. We examine ED disposition of PLwD compared with older adults with non-dementia chronic disease as well as healthcare utilization and survival.
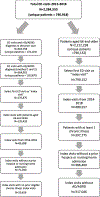
Methods: Medicare claims data were used to identify community-dwelling older adults 66+ years old from 34 hospitals with either Alzheimer's disease/Alzheimer's disease related dementias (AD/ADRD) or a non-AD/ADRD chronic condition between January 1, 2014, and December 31, 2018. We compared ED disposition at the index visit, as well as healthcare utilization and mortality in the 12 months following an index ED visit, and adjusted for age, gender, and risk of mortality.
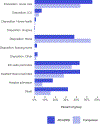
Results: There were 29,626 patients in the AD/ADRD sample, and 317,046 in the comparison sample. The AD/ADRD sample was older (82.4 years old [SD: 8.2] vs. 76.0 years old [SD: 7.7]) and had more female patients (59.9% vs. 54.7%). The AD/ADRD sample was more likely to experience ED disposition to acute care (OR 1.039, p < 0.001, 95% CI 1.029-1.050), to have an ED revisit (OR 1.077, p < 0.001, 95% CI 1.066-1.087), and an inpatient stay in the subsequent 12 months (OR 1.085, p < 0.001, 95% CI 1.075-1.095). ED disposition to hospice was low in both samples (0.2%). AD/ADRD patients had a higher risk of mortality (OR 1.099, p < 0.001, 95% CI 1.091-1.107) and high short-term mortality (31.9% within 12 months) than those without AD/ADRD (15.3% within 12 months).
Conclusions: PLwD who visit the ED have high short-term mortality. Despite this, disposition to acute care, ED revisits, and inpatient stays, rather than hospice, remain the predominant mode of care delivery. Transition directly from the ED to hospice for PLwD is rare.
Keywords: Alzheimer's disease; Medicare; emergency medicine; geriatrics; healthcare utilization.
© 2022 The American Geriatrics Society.
Conflict of interest statement
Conflict of Interest
The authors have no conflicts of interest to declare.
Figures
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

