Prevalence of Oropharyngeal Dysphagia in Adults in Different Healthcare Settings: A Systematic Review and Meta-analyses
- PMID: 35639156
- PMCID: PMC9873728
- DOI: 10.1007/s00455-022-10465-x
Prevalence of Oropharyngeal Dysphagia in Adults in Different Healthcare Settings: A Systematic Review and Meta-analyses
Abstract
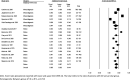
Oropharyngeal dysphagia (OD) is prevalent in the elderly and persons with complex medical conditions, resulting in considerable medical and psychosocial consequences and reduced quality of life. Many prevalence studies regard OD in relation to age or diagnosis. Knowledge on the prevalence of OD in different healthcare settings is lacking. This systematic review aimed to estimate the prevalence of OD in adults admitted to hospitals, rehabilitation facilities, nursing homes, and palliative care facilities through meta-analyses. A systematic literature search was completed including all dates up to March 30, 2021. The methodology and reporting were based on the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA). Forty-four out of 1,956 screened articles were deemed eligible. Considerable heterogeneity in definitions of OD and type and quality of selected outcome measures were observed. Overall within-group pooled prevalence estimates for OD determined by meta-analysis were 36.5% (95% CI 29.9 - 43.6) in the hospital setting, 42.5% (95% CI 35.8 - 49.5) in the rehabilitation setting, and 50.2% (95% CI 33.3-67.2) in nursing homes. No OD prevalence data were identified for palliative care facilities. Results for between-group analyses of OD prevalence estimates in the hospital setting were non-significant for type of assessment method, diagnostic group, and type of hospital ward, but indicated significantly higher prevalence estimates in nursing homes when using screening compared to patient-report. Future research should provide OD prevalence data for palliative care, achieve consensus in OD-related terminology when performing prevalence studies, and use screening and assessments with optimal diagnostic performance and psychometric properties.
Keywords: Deglutition; Hospital; Nursing home; Prevalence; Rehabilitation; Swallowing disorders.
© 2022. The Author(s).
Conflict of interest statement
The authors have no relevant financial or non-financial interests to disclose.
Figures





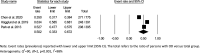

References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

