Advances in Regenerative Sports Medicine Research
- PMID: 35646865
- PMCID: PMC9136559
- DOI: 10.3389/fbioe.2022.908751
Advances in Regenerative Sports Medicine Research
Erratum in
-
Corrigendum: Advances in regenerative sports medicine research.Front Bioeng Biotechnol. 2022 Sep 23;10:1035342. doi: 10.3389/fbioe.2022.1035342. eCollection 2022. Front Bioeng Biotechnol. 2022. PMID: 36213056 Free PMC article.
Abstract
Regenerative sports medicine aims to address sports and aging-related conditions in the locomotor system using techniques that induce tissue regeneration. It also involves the treatment of meniscus and ligament injuries in the knee, Achilles' tendon ruptures, rotator cuff tears, and cartilage and bone defects in various joints, as well as the regeneration of tendon-bone and cartilage-bone interfaces. There has been considerable progress in this field in recent years, resulting in promising steps toward the development of improved treatments as well as the identification of conundrums that require further targeted research. In this review the regeneration techniques currently considered optimal for each area of regenerative sports medicine have been reviewed and the time required for feasible clinical translation has been assessed. This review also provides insights into the direction of future efforts to minimize the gap between basic research and clinical applications.
Keywords: bone; cartilage; meniscus; regenerative medicine; rotator cuff; sports medicine; tendon-to-bone.
Copyright © 2022 Wang, Jiang, Lin, Zhu, Cai, Su, Chen, Xu, Li, Wang, Zhang and Zhao.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest. The handling editor, KL, and Reviewer, XY, declared a shared parent affiliation with the authors LW, JJ, JC, WS, JCh, JX, YL, JW, JZ, at the time of review.
Figures


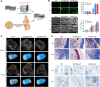

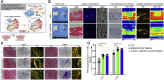
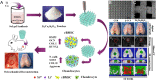


References
-
- Ai C., Sheng D., Chen J., Cai J., Wang S., Jiang J., et al. (2017). Surface Modification of Vascular Endothelial Growth Factor-Loaded Silk Fibroin to Improve Biological Performance of Ultra-high-molecular-weight Polyethylene via Promoting Angiogenesis. Int. J. Nanomedicine 12. 10.2147/IJN.S148845 - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

