Pre-hospital exposures to antibiotics among children presenting with fever in northern Uganda: a facility-based cross-sectional study
- PMID: 35650548
- PMCID: PMC9157045
- DOI: 10.1186/s12887-022-03375-2
Pre-hospital exposures to antibiotics among children presenting with fever in northern Uganda: a facility-based cross-sectional study
Abstract
Background: The rise in the indiscriminate use of antibiotics has become a major global public health problem and presents the biggest global health challenge in the twenty-first century. In developing countries, caregivers initiate treatment with antibiotics at home before presentation to a health facility. However, there is a paucity of evolving data towards surveillance of this trend in low-income countries. We investigated antibiotic use among febrile children presenting to a tertiary health facility in northern Uganda.
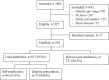
Methods: We conducted a cross-sectional study in a tertiary health facility in northern Uganda between March and September 2021. Children aged 6-59 months with fever were selected using systematic random sampling. A pre-tested interviewer-administered questionnaire was used the collect clinical data from the caregivers. Data were analyzed using SPSS version 23. Descriptive statistics and multiple logistic regression models were applied. P-value < 0.05 was considered for statistical significance.
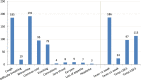
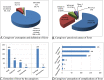
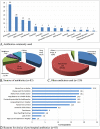
Results: Eighty-three (39.5%) of the 210 children with fever in this study used antibiotics prior to the hospital visit, 55.4% of which were on a self-medication basis, while 44.6% were empiric prescriptions. The most commonly used antibiotics were amoxicillin 33/83 (39.8%), erythromycin 18 (21.7%), metronidazole 14 (16.9%), ciprofloxacin 13 (15.7%) and ampicillin 6 (7.2%). The main sources of the antibiotics included buying from drug shops 30/83 (36.1%), issuance from clinics (33.7%), remnants at home (12.0%), picking from a neighbour (7.2%) and others (10.8%). The factors associated with antibiotic use among the febrile children were residence (p < 0.001); distance from the nearest health facility (p = 0.005); caregivers' gender (p = 0.043); cough (p = 0.012); diarrhoea (p = 0.007); duration of fever (p = 0.002); perceived convulsion complicating fever (p = 0.026), and caregivers' perception that fever (p = 0.001), cough (p = 0.003), diarrhoea (p < 0.001) and any infection (p < 0.001) are indications for antibiotics.
Conclusions: Inappropriate use of antibiotics for childhood febrile illnesses is prevalent in the study setting, facilitated by the ease of access and use of leftover antibiotics. There is a need to address communities' health-seeking behaviour and the health providers' practice alike.
Keywords: Antibiotic; Antimicrobial resistance; Children; Fever.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
Similar articles
-
Antibiotics Self Medication among Children: A Systematic Review.Antibiotics (Basel). 2022 Nov 9;11(11):1583. doi: 10.3390/antibiotics11111583. Antibiotics (Basel). 2022. PMID: 36358240 Free PMC article. Review.
-
Anti-malarial drug use, appropriateness and associated factors among children under-five with febrile illnesses presenting to a tertiary health facility: a cross sectional study.Malar J. 2023 Mar 21;22(1):103. doi: 10.1186/s12936-023-04534-1. Malar J. 2023. PMID: 36941616 Free PMC article.
-
Antibiotic exposure among children younger than 5 years in low-income and middle-income countries: a cross-sectional study of nationally representative facility-based and household-based surveys.Lancet Infect Dis. 2020 Feb;20(2):179-187. doi: 10.1016/S1473-3099(19)30572-9. Epub 2019 Dec 13. Lancet Infect Dis. 2020. PMID: 31843383
-
Validity of caregivers' reports on prior use of antibacterials in children under five years presenting to health facilities in Gulu, northern Uganda.PLoS One. 2021 Sep 16;16(9):e0257328. doi: 10.1371/journal.pone.0257328. eCollection 2021. PLoS One. 2021. PMID: 34529730 Free PMC article.
-
The nature of self-medication in Uganda: a systematic review and meta-analysis.BMC Public Health. 2025 Jan 17;25(1):197. doi: 10.1186/s12889-025-21380-9. BMC Public Health. 2025. PMID: 39825271 Free PMC article.
Cited by
-
Non-prescribed antibiotic use for children at community levels in low- and middle-income countries: a systematic review and meta-analysis.J Pharm Policy Pract. 2022 Sep 30;15(1):57. doi: 10.1186/s40545-022-00454-8. J Pharm Policy Pract. 2022. PMID: 36180895 Free PMC article.
-
Non-prescription antibiotic use and its predictors among children in low- and middle-income countries: a systematic review and meta-analysis.Ital J Pediatr. 2024 Dec 18;50(1):260. doi: 10.1186/s13052-024-01808-5. Ital J Pediatr. 2024. PMID: 39696454 Free PMC article.
-
Antibiotic prescription from qualified sources for children with fever/cough: cross-sectional study from 59 low- and middle-income countries.EClinicalMedicine. 2023 Jun 29;61:102055. doi: 10.1016/j.eclinm.2023.102055. eCollection 2023 Jul. EClinicalMedicine. 2023. PMID: 37434742 Free PMC article.
-
Status and implications of the knowledge, attitudes and practices towards AWaRe antibiotic use, resistance and stewardship among low- and middle-income countries.JAC Antimicrob Resist. 2025 Mar 25;7(2):dlaf033. doi: 10.1093/jacamr/dlaf033. eCollection 2025 Apr. JAC Antimicrob Resist. 2025. PMID: 40134815 Free PMC article. Review.
-
Antibiotics Self Medication among Children: A Systematic Review.Antibiotics (Basel). 2022 Nov 9;11(11):1583. doi: 10.3390/antibiotics11111583. Antibiotics (Basel). 2022. PMID: 36358240 Free PMC article. Review.
References
-
- Katarina Ilić’s, Vesna Škodrić-Trifunović’s: Social-economic factors and irrational antibiotic use as reasons for antibiotic resistance of bacteria causing common childhood infections in primary healthcare. Eur J Pediatr. 2012;171:767–777. 10.1007/s00431-00011-01592-00435. - PubMed
-
- World Health Organization. WHO Policy Perspectives on Medicines- Promoting rational use of medicines: core components. Geneva: World Health Organization; 2002. available at: https://apps.who.int/iris/bitstream/handle/10665/67438/WHO_EDM_2002.3.pdf.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical