Association between early cumulative fluid balance and successful liberation from invasive ventilation in COVID-19 ARDS patients - insights from the PRoVENT-COVID study: a national, multicenter, observational cohort analysis
- PMID: 35650616
- PMCID: PMC9157033
- DOI: 10.1186/s13054-022-04023-y
Association between early cumulative fluid balance and successful liberation from invasive ventilation in COVID-19 ARDS patients - insights from the PRoVENT-COVID study: a national, multicenter, observational cohort analysis
Abstract
Background: Increasing evidence indicates the potential benefits of restricted fluid management in critically ill patients. Evidence lacks on the optimal fluid management strategy for invasively ventilated COVID-19 patients. We hypothesized that the cumulative fluid balance would affect the successful liberation of invasive ventilation in COVID-19 patients with acute respiratory distress syndrome (ARDS).
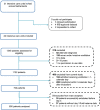
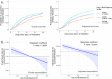
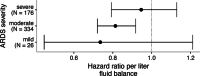
Methods: We analyzed data from the multicenter observational 'PRactice of VENTilation in COVID-19 patients' study. Patients with confirmed COVID-19 and ARDS who required invasive ventilation during the first 3 months of the international outbreak (March 1, 2020, to June 2020) across 22 hospitals in the Netherlands were included. The primary outcome was successful liberation of invasive ventilation, modeled as a function of day 3 cumulative fluid balance using Cox proportional hazards models, using the crude and the adjusted association. Sensitivity analyses without missing data and modeling ARDS severity were performed.
Results: Among 650 patients, three groups were identified. Patients in the higher, intermediate, and lower groups had a median cumulative fluid balance of 1.98 L (1.27-7.72 L), 0.78 L (0.26-1.27 L), and - 0.35 L (- 6.52-0.26 L), respectively. Higher day 3 cumulative fluid balance was significantly associated with a lower probability of successful ventilation liberation (adjusted hazard ratio 0.86, 95% CI 0.77-0.95, P = 0.0047). Sensitivity analyses showed similar results.
Conclusions: In a cohort of invasively ventilated patients with COVID-19 and ARDS, a higher cumulative fluid balance was associated with a longer ventilation duration, indicating that restricted fluid management in these patients may be beneficial. Trial registration Clinicaltrials.gov ( NCT04346342 ); Date of registration: April 15, 2020.
Keywords: ARDS; COVID-19; Critical care; Cumulative fluid balance; Liberation of ventilation.
© 2022. The Author(s).
Conflict of interest statement
All authors declare no competing interests related to the submitted work.
Figures
Comment in
-
Fluid intake, fluid output or fluid balance, which one matters in ARDS.Crit Care. 2022 Nov 14;26(1):352. doi: 10.1186/s13054-022-04188-6. Crit Care. 2022. PMID: 36376940 Free PMC article. No abstract available.
References
-
- Hasan SS, Capstick T, Ahmed R, Kow CS, Mazhar F, Merchant HA, Zaidi STR. Mortality in COVID-19 patients with acute respiratory distress syndrome and corticosteroids use: a systematic review and meta-analysis. Expert Rev Respir Med. 2020;14(11):1149–1163. doi: 10.1080/17476348.2020.1804365. - DOI - PMC - PubMed
-
- van Mourik N, Metske HA, Hofstra JJ, Binnekade JM, Geerts BF, Schultz MJ, Vlaar APJ. Cumulative fluid balance predicts mortality and increases time on mechanical ventilation in ARDS patients: an observational cohort study. PLoS ONE. 2019;14(10):e0224563. doi: 10.1371/journal.pone.0224563. - DOI - PMC - PubMed
-
- Alhazzani W, Moller MH, Arabi YM, Loeb M, Gong MN, Fan E, Oczkowski S, Levy MM, Derde L, Dzierba A, et al. Surviving Sepsis Campaign: guidelines on the management of critically ill adults with Coronavirus Disease 2019 (COVID-19) Intensive Care Med. 2020;46(5):854–887. doi: 10.1007/s00134-020-06022-5. - DOI - PMC - PubMed
-
- Silversides JA, Major E, Ferguson AJ, Mann EE, McAuley DF, Marshall JC, Blackwood B, Fan E. Conservative fluid management or deresuscitation for patients with sepsis or acute respiratory distress syndrome following the resuscitation phase of critical illness: a systematic review and meta-analysis. Intensive Care Med. 2017;43(2):155–170. doi: 10.1007/s00134-016-4573-3. - DOI - PubMed
-
- National Heart L, Blood Institute Acute Respiratory Distress Syndrome Clinical Trials N, Wiedemann HP, Wheeler AP, Bernard GR, Thompson BT, Hayden D, deBoisblanc B, Connors AF Jr., Hite RD et al. Comparison of two fluid-management strategies in acute lung injury. N Engl J Med. 2006;354(24):2564–75. - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

