A scoping review: virtual patients for communication skills in medical undergraduates
- PMID: 35659213
- PMCID: PMC9166208
- DOI: 10.1186/s12909-022-03474-9
A scoping review: virtual patients for communication skills in medical undergraduates
Abstract
Background: Communication is an essential competence for medical students. Virtual patients (VP), computerized educational tools where users take the role of doctor, are increasingly used. Despite the wide range of VP utilization, evidence-based practical guidance on supporting development of communication skills for medical students remains unclear. We focused this scoping review on VP affordance for student learning especially important in the current environment of constrained patient access.
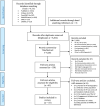
Methods: This scoping review followed Arksey & O'Malley's methodology. We tested and used a search strategy involving six databases, resulting in 5,262 citations. Two reviewers independently screened titles, full texts (n= 158) and finally performed data extraction on fifty-five included articles. To support consideration of educational affordance the authors employed a pragmatic framework (derived from activity theory) to map included studies on VP structure, curricular alignment, mediation of VP activity, and socio-cultural context.
Results: Findings suggest that not only the VP itself, but also its contextualization and associated curricular activities influence outcomes. The VP was trialled in the highest proportion of papers as a one-off intervention (19 studies), for an average duration of 44.9 minutes (range 10-120min), mainly in senior medical students (n=23), notably the largest group of studies did not have VP activities with explicit curricular integration (47%). There was relatively little repeated practice, low levels of feedback, self-reflection, and assessment. Students viewed VPs overall, citing authenticity and ease of use as important features. Resource implications are often omitted, and costings would facilitate a more complete understanding of implications of VP use.
Conclusion: Students should be provided with maximal opportunity to draw out the VPs' full potential through repeated practice, without time-constraint and with curricular alignment. Feedback delivery enabling reflection and mastery is also key. The authors recommend educators to explicitly balance computerized authenticity with instructional design integrated within the curriculum.
Keywords: Communication skills; Consultation skills; Medical students; Online medical teaching; Technology enhanced learning; Undergraduate; Virtual Patients; Virtual learning.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
References
-
- O'Daniel M, Rosentein A. Patient Safety and Quality: An evidence-based handbook for Nurses: Vol 2. USA: Hughes, RG; 2008. Chapter 33: Professional Communication and Team Collaboration.
-
- Merten H, van Galen LS, Wagner C. Safe Handover. Br Med J. 2017:1–5. - PubMed
-
- Association of Amercian Colleges. Recommendations for clinical skills curricula for undergraduate medical education: AAMC; 2005. [Online]:Available at: https://store.aamc.org/downloadable/download/sample/sample_id/174/ [Accessed 24 Nov 2019]
-
- Irish Medical Council. Guide to Professional Conduct and Ethics for Registered Medical Practitioners (Amended). 8th Edition [online]. ed. Dublin: Irish Medical Council; 2019. - PubMed
-
- General Medical Council. Good Medical Practice [online]. UK: General Medical Council; 2019.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources