Mechanisms of ductular reaction in non-alcoholic steatohepatitis
- PMID: 35664038
- PMCID: PMC9134136
- DOI: 10.3748/wjg.v28.i19.2088
Mechanisms of ductular reaction in non-alcoholic steatohepatitis
Abstract
Non-alcoholic fatty liver disease (NAFLD) is a disease spectrum caused in part by insulin resistance and genetic predisposition. This disease is primarily characterized by excessive lipid accumulation in hepatocytes in the absence of alcohol abuse and other causes of liver damage. Histologically, NAFLD is divided into several periods: simple steatosis, non-alcoholic steatohepatitis (NASH), hepatic fibrosis, cirrhosis, and hepatocellular carcinoma. With the increasing prevalence of obesity and hyperlipidemia, NAFLD has become the main cause of chronic liver disease worldwide. As a result, the pathogenesis of this disease is drawing increasing attention. Ductular reaction (DR) is a reactive bile duct hyperplasia caused by liver injury that involves hepatocytes, cholangiocytes, and hepatic progenitor cells. Recently, DR is shown to play a pivotal role in simple steatosis progression to NASH or liver fibrosis, providing new research and treatment options. This study reviews several DR signaling pathways, including Notch, Hippo/YAP-TAZ, Wnt/β-catenin, Hedgehog, HGF/c-Met, and TWEAK/Fn14, and their role in the occurrence and development of NASH.
Keywords: Ductular reaction; Mechanisms; Non-alcoholic fatty liver disease; Non-alcoholic steatohepatitis; Signaling pathways.
©The Author(s) 2022. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: The authors declare no conflict of interest for this article.
Figures
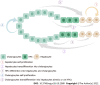
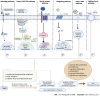
References
-
- Younossi ZM, Koenig AB, Abdelatif D, Fazel Y, Henry L, Wymer M. Global epidemiology of nonalcoholic fatty liver disease-Meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology . 2016;64:73–84. - PubMed
-
- Li J, Zou B, Yeo YH, Feng Y, Xie X, Lee DH, Fujii H, Wu Y, Kam LY, Ji F, Li X, Chien N, Wei M, Ogawa E, Zhao C, Wu X, Stave CD, Henry L, Barnett S, Takahashi H, Furusyo N, Eguchi Y, Hsu YC, Lee TY, Ren W, Qin C, Jun DW, Toyoda H, Wong VW, Cheung R, Zhu Q, Nguyen MH. Prevalence, incidence, and outcome of non-alcoholic fatty liver disease in Asia, 1999-2019: a systematic review and meta-analysis. Lancet Gastroenterol Hepatol . 2019;4:389–398. - PubMed
-
- Rinella ME. Nonalcoholic fatty liver disease: a systematic review. JAMA . 2015;313:2263–2273. - PubMed
-
- Dezső K, Nagy P, Paku S. Human liver regeneration following massive hepatic necrosis: Two distinct patterns. J Gastroenterol Hepatol . 2020;35:124–134. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

