The effect of national antenatal care guidelines and provider training on obstetric danger sign counselling: a propensity score matching analysis of the 2014 Ethiopia service provision assessment plus survey
- PMID: 35668529
- PMCID: PMC9167913
- DOI: 10.1186/s12978-022-01442-6
The effect of national antenatal care guidelines and provider training on obstetric danger sign counselling: a propensity score matching analysis of the 2014 Ethiopia service provision assessment plus survey
Erratum in
-
Correction: The effect of national antenatal care guidelines and provider training on obstetric danger sign counselling: a propensity score matching analysis of the 2014 Ethiopia service provision assessment plus survey.Reprod Health. 2022 Aug 17;19(1):179. doi: 10.1186/s12978-022-01483-x. Reprod Health. 2022. PMID: 35978357 Free PMC article. No abstract available.
Abstract
Background: Most pregnant women in low and lower-middle-income countries do not receive all components of antenatal care (ANC), including counselling on obstetric danger signs. Facility-level ANC guidelines and provider in-service training are major factors influencing ANC counselling. In Ethiopia, little is known about the extent to which guidelines and provider in-service training can increase the quality of ANC counselling.
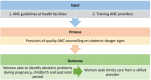
Methods: We examined the effect of national ANC guidelines and ANC provider in-service training on obstetric danger sign counselling for pregnant women receiving ANC using the 2014 Ethiopian service provision assessment plus (ESPA +) survey data. We created two analysis samples by applying a propensity score matching method. The first sample consisted of women who received ANC at health facilities with guidelines matched with those who received ANC at health facilities without guidelines. The second sample consisted of women who received ANC from the providers who had undertaken in-service training in the last 24 months matched with women who received ANC from untrained providers. The outcome variable was the number of obstetric danger signs described during ANC counselling, ranging from zero to eight. The covariates included women's socio-demographic characteristics, obstetric history, health facility characteristics, and ANC provider characteristics.
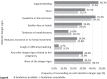
Results: We found that counselling women about obstetric danger signs during their ANC session varied according to the availability of ANC guidelines (61% to 70%) and provider training (62% to 68%). After matching the study participants by the measured covariates, the availability of ANC guidelines at the facility level significantly increased the average number of obstetric danger signs women received during counselling by 24% (95% CI: 12-35%). Similarly, providing refresher training for ANC providers increased the average number of obstetric danger signs described during counselling by 37% (95% CI: 26-48%).
Conclusion: The findings suggest that the quality of ANC counselling in Ethiopia needs strengthening by ensuring that ANC guidelines are available at every health facility and that the providers receive regular ANC related in-service training.
Keywords: Antenatal care; Counselling; Obstetric danger signs.
Plain language summary
Maternal death from preventable pregnancy-related complications remains a global health challenge. In 2017, there were 295,000 maternal deaths worldwide, and about two-thirds of these deaths were from Sub-Saharan Africa. Ethiopia is a Sub-Saharan African country with 401 maternal deaths per 100,000 live births in 2017, and this rate is higher than the target indicated in sustainable development goals. Most maternal deaths are due to obstetric complications and could have been averted through early detection and treatment. Providing antenatal care counselling about obstetric danger signs enhances women’s awareness of obstetric complications and encourages women to seek treatment from a skilled care provider. However, most women from low-income settings, including Ethiopia, do not receive counselling about obstetric danger signs. Facility-level antenatal care guidelines and provider in-service training improve antenatal care counselling. In Ethiopia, little is known to what extent antenatal care guidelines and provider training increase counselling on obstetric danger signs. The present study used the 2014 Ethiopian service provision assessment data and estimated the effect of antenatal care guidelines and provider training on counselling about obstetric danger signs. The analysis involved a propensity score matching method and included 1725 pregnant women. The study found that antenatal care guidelines at health facilities and antenatal care provider in-service training significantly increase counselling on obstetric danger signs by 24% and 37%, respectively. The finding suggests improving the quality of antenatal care counselling in Ethiopia needs antenatal care guidelines at each antenatal care clinic and refresher training for the providers.
© 2022. The Author(s).
Conflict of interest statement
The authors have declared no conflict of interest.
Figures


References
-
- WHO. WHO: recommended definitions, terminology and format for statistical tables related to the perinatal period and use of a new certificate for cause of perinatal deaths. Modifications recommended by FIGO as amended October 14, 1976. Acta Obstet Gynecol Scand. 1977;56(3):247-53. - PubMed
-
- WHO. Trends in maternal mortality 2000 to 2017: estimates by WHO, UNICEF, UNFPA, World Bank Group and the United Nations Population Division: executive summary.; 2019.
-
- WHO. World Health Statistics 2020. Geneva: WHO; 2021.
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

