State-of-the-art imaging in oesophago-gastric cancer
- PMID: 35671095
- PMCID: PMC10996959
- DOI: 10.1259/bjr.20220410
State-of-the-art imaging in oesophago-gastric cancer
Abstract
Radiological investigations are essential in the management of oesophageal and gastro-oesophageal junction cancers. The current multimodal combination of CT, 18F-fluorodeoxyglucose positron emission tomography combined with CT (PET/CT) and endoscopic ultrasound (EUS) has limitations, which hinders the prognostic and predictive information that can be used to guide optimum treatment decisions. Therefore, the development of improved imaging techniques is vital to improve patient management. This review describes the current evidence for state-of-the-art imaging techniques in oesophago-gastric cancer including high resolution MRI, diffusion-weighted MRI, dynamic contrast-enhanced MRI, whole-body MRI, perfusion CT, novel PET tracers, and integrated PET/MRI. These novel imaging techniques may help clinicians improve the diagnosis, staging, treatment planning, and response assessment of oesophago-gastric cancer.
Figures

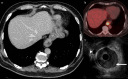
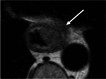

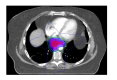
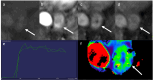
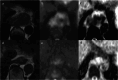
References
-
- Cancer Research . Oesophageal cancer incidence statistics . Available from : https://www.cancerresearchuk.org/health-professional/cancer-statistics/s...
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

