Enterococcus faecium and Pediococcus acidilactici deteriorate Enterobacteriaceae-induced depression and colitis in mice
- PMID: 35672451
- PMCID: PMC9174183
- DOI: 10.1038/s41598-022-13629-9
Enterococcus faecium and Pediococcus acidilactici deteriorate Enterobacteriaceae-induced depression and colitis in mice
Erratum in
-
Author Correction: Enterococcus faecium and Pediococcus acidilactici deteriorate Enterobacteriaceae-induced depression and colitis in mice.Sci Rep. 2023 Aug 10;13(1):12997. doi: 10.1038/s41598-023-39969-8. Sci Rep. 2023. PMID: 37563202 Free PMC article. No abstract available.
Abstract
Gut dysbiosis is closely associated with the outbreak of inflammatory bowel disease (IBD) and psychiatric disorder. The Enterobacteriaceae population was higher in the feces of patients with inflammatory bowel disease (IBD-F) than in those of healthy control volunteers (HC-F). The Enterococcaceae and Lactobacillaceae populations were higher in the feces of IBD patients with depression (IBD/D+-F) vs. the feces of IBD patients without depression (IBD/D--F). Therefore, we examined the effects of Klebsiella oxytoca, Escherichia coli, Cronobacter sakazakii, Enterococcus faecium, and Pediococcus acidolactici overpopulated in IBD/D+-F and their byproducts LPS and exopolysaccharide (EPS) on the occurrence of depression and colitis in mice. Oral gavages of Klebsiella oxytoca, Escherichia coli, and Cronobacter sakazakii belonging to Enterobacteriaceae, singly or together, caused dose-dependently colitis and depression-like behaviors in germ-free and specific-pathogen-free mice. Although Enterococcus faecium and Pediococcus acidolactici did not significantly cause colitis and depression-like behaviors, they significantly deteriorated Klebsiella oxytoca- or Escherichia coli-induced colitis, neuroinflammation, and anxiety/depression-like behaviors and increased blood LPS, corticosterone, and IL-6 levels. The EPSs from Enterococcus faecium and Pediococcus acidolactici also worsened Klebsiella oxytoca LPS-induced colitis, neuroinflammation, and depression-like behaviors in mice and increased the translocation of fluorescein isothiocyanate-conjugated LPS into the hippocampus. However, Bifidobacterium longum, which was lower in IBD/D+-F vs. IBD/D--F, or its EPS suppressed them. In conclusion, Enterococcus faecium and Pediococcus acidolactici, known as a probiotic strain, and their EPSs may be a risk factor for the outbreak of depression and IBD.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures






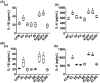
Similar articles
-
Transplantation of fecal microbiota from patients with inflammatory bowel disease and depression alters immune response and behavior in recipient mice.Sci Rep. 2021 Oct 14;11(1):20406. doi: 10.1038/s41598-021-00088-x. Sci Rep. 2021. PMID: 34650107 Free PMC article.
-
The Alleviation of Gut Microbiota-Induced Depression and Colitis in Mice by Anti-Inflammatory Probiotics NK151, NK173, and NK175.Nutrients. 2022 May 16;14(10):2080. doi: 10.3390/nu14102080. Nutrients. 2022. PMID: 35631220 Free PMC article.
-
Overrepresentation of Enterobacteriaceae and Escherichia coli is the major gut microbiome signature in Crohn's disease and ulcerative colitis; a comprehensive metagenomic analysis of IBDMDB datasets.Front Cell Infect Microbiol. 2022 Oct 4;12:1015890. doi: 10.3389/fcimb.2022.1015890. eCollection 2022. Front Cell Infect Microbiol. 2022. PMID: 36268225 Free PMC article.
-
Probiotics and Their Use in Inflammatory Bowel Disease.Altern Ther Health Med. 2018 May;24(3):16-23. Altern Ther Health Med. 2018. PMID: 29135456 Review.
-
Interrelatedness between dysbiosis in the gut microbiota due to immunodeficiency and disease penetrance of colitis.Immunology. 2015 Nov;146(3):359-68. doi: 10.1111/imm.12511. Epub 2015 Sep 7. Immunology. 2015. PMID: 26211540 Free PMC article. Review.
Cited by
-
Probiotic mitigates gut hypoperfusion-associated acute gastrointestinal injury in patients undergoing cardiopulmonary bypass: a randomized controlled trial.BMC Med. 2025 Apr 23;23(1):238. doi: 10.1186/s12916-025-04082-2. BMC Med. 2025. PMID: 40264088 Free PMC article. Clinical Trial.
-
Gut microbiome and peritoneal inflammation: a new perspective on peritoneal dialysis-associated peritonitis.Ren Fail. 2025 Dec;47(1):2542532. doi: 10.1080/0886022X.2025.2542532. Epub 2025 Aug 7. Ren Fail. 2025. PMID: 40775606 Free PMC article.
-
Lactococcus lactis and Bifidobacterium bifidum alleviate postmenopausal symptoms by suppressing NF-κB signaling and microbiota dysbiosis.Sci Rep. 2024 Dec 30;14(1):31675. doi: 10.1038/s41598-024-81500-0. Sci Rep. 2024. PMID: 39738244 Free PMC article.
-
Preconception maternal gut dysbiosis affects enteric nervous system development and disease susceptibility in offspring via the GPR41-GDNF/RET/SOX10 signaling pathway.Imeta. 2025 Mar 18;4(2):e70012. doi: 10.1002/imt2.70012. eCollection 2025 Apr. Imeta. 2025. PMID: 40236770 Free PMC article.
-
Periodontitis salivary microbiota exacerbates colitis-induced anxiety-like behavior via gut microbiota.NPJ Biofilms Microbiomes. 2023 Dec 7;9(1):93. doi: 10.1038/s41522-023-00462-9. NPJ Biofilms Microbiomes. 2023. PMID: 38062089 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

