Chronic CSF leak from lumbar-peritoneal shunt tract: A case report
- PMID: 35673636
- PMCID: PMC9168392
- DOI: 10.25259/SNI_1084_2021
Chronic CSF leak from lumbar-peritoneal shunt tract: A case report
Abstract
Background: We describe a case of long-standing intracranial hypotension caused by an iatrogenic arachnoid diverticulum. This case illustrates two learning points. First, excessive CSF absorption may occur through an acquired arachnoid-epidural venous plexus at a dural defect. Second, a long-standing CSF leak may benefit from definitive surgical repair in the first instance.
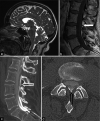
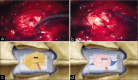
Case description: A 55-year-old female, with known idiopathic intracranial hypertension, presented with disabling chronic low-pressure symptoms after having a lumboperitoneal shunt removed 5 years previously. MRI scan revealed a Chiari I malformation (CMI) and a small dural interruption at the L3/4 space. CT myelography confirmed the abnormality. Intraoperatively, a dural defect and arachnoid bleb with an overlying attachment of adipose tissue and a vessel were found. Postoperatively, the patient has marked resolution of her headaches and dizziness and is mobilizing independently.
Conclusion: Excessive CSF absorption appears to have occurred through an acquired arachnoid-epidural venous plexus. A high index of suspicion for intracranial hypotension is required in patients with low pressure symptoms and a CMI.
Keywords: CSF; Chiari; Intracranial hypotension; Shunt; Spine.
Copyright: © 2022 Surgical Neurology International.
Conflict of interest statement
There are no conflicts of interest.
Figures
References
-
- Abrishamkar S, Khalighinejad N, Moein P. Analysing the effect of early acetazolamide administration on patients with a high risk of permanent cerebrospinal fluid leakage. Acta Med Iran. 2013;51:467–71. - PubMed
-
- Atkinson JL, Weinshenker BG, Miller GM, Piepgras DG, Mokri B. Acquired Chiari I malformation secondary to spontaneous spinal cerebrospinal fluid leakage and chronic intracranial hypotension syndrome in seven cases. J Neurosurg. 1998;88:237–42. - PubMed
-
- Brodbelt A, Stoodley M. CSF pathways: A review. Br J Neurosurg. 2007;21:510–20. - PubMed
-
- Chumas PD, Armstrong DC, Drake JM, Kulkarni AV, Hoffman HJ, Humphreys RP, et al. Tonsillar herniation: The rule rather than the exception after lumboperitoneal shunting in the pediatric population. J Neurosurg. 1993;78:568–73. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
