Clinical and immunohistopathological study of conjunctival melanocytic lesions in pediatric and adolescent patients. A case series
- PMID: 35673810
- PMCID: PMC9289701
- DOI: 10.47162/RJME.62.4.03
Clinical and immunohistopathological study of conjunctival melanocytic lesions in pediatric and adolescent patients. A case series
Abstract
Background: Conjunctival pigmented neoplasia can be benign, premalignant or malignant tumors. Our study aims to establish the epidemiological, gross morphological and immunohistopathological features of the conjunctival pigmented lesions in pediatric and adolescent patients (<18 years), to establish an accurate diagnosis.
Patients, material and methods: This is a retrospective case series study conducted within two Ophthalmology Clinics from Iaşi, Romania, on seven pediatric and adolescent patients. Using the Clinical Observation Chart and the Pathology Registers over a six-years period (January 2015-December 2021), we noted the patients' demographic data, clinical data, and ophthalmological investigations of the lesion, as well as the type of their treatment. All histological sections stained with Hematoxylin-Eosin (HE) and with five antibodies [pan-cytokeratin (pan-CK) AE1∕AE3, S100 protein, Melan A, human melanoma black 45 (HMB45), and Ki67] were re-examined by four pathologists for each case, to identify the type of the conjunctival lesion and its histological and immunohistochemical features.
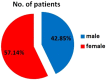
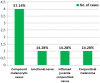
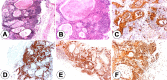
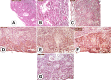
Results: The mean age of all patients was 10.28 years, and the female∕male ratio was 1.3. Right eye was more often affected (71.42%). 71.42% of cases presented an elevated lesion, 57.14% of cases showed a lightly pigmented lesion, but 14.28% of cases exhibited a pink lesion and this feature described the inflamed juvenile conjunctival nevus. In all cases (100%) the conjunctival pigmented tumor was removed with safety margins. The microscopic examination revealed a compound melanocytic nevus in 57.14% cases, a junctional conjunctival nevus in 14.28% cases, an inflamed juvenile nevus in 14.28% cases, and a conjunctival melanoma arising from a pre-existing nevus in 14.28% cases. In all cases of nevi, the nevoid melanocytes showed strong immunopositivity for Melan A and S100 protein, variable and weak immunopositivity for HMB45, and a mean Ki67 labeling index of 1.71%. Conjunctival melanoma revealed strong immunopositivity of tumor cells for HMB45, Melan A and S100 protein, and a Ki67 labeling index of 20%. In all cases, the conjunctival epithelium showed strong immunopositivity for pan-CK AE1∕AE3. All our cases (100%) had a favorable outcome after the surgical removal of the tumor.
Conclusions: Any excision of a conjunctival pigmented lesion must be subject to a systematic immunohistopathological examination, and there is a set of antibodies (anti-HMB45 and anti-Ki67) that are useful for differential diagnosis between a conjunctival nevus and a conjunctival melanoma.
Conflict of interest statement
The authors declare that they have no conflict of interests.
Figures

Similar articles
-
Immunohistochemical analysis of benign and malignant melanocytic lesions of the conjunctiva using double-staining.Can J Ophthalmol. 2019 Dec;54(6):699-707. doi: 10.1016/j.jcjo.2019.03.015. Epub 2019 Jun 14. Can J Ophthalmol. 2019. PMID: 31836103
-
WT1 and Bcl2 expression in melanocytic lesions of the conjunctiva: an immunohistochemical study of 123 cases.Arch Ophthalmol. 2009 Aug;127(8):964-9. doi: 10.1001/archophthalmol.2009.183. Arch Ophthalmol. 2009. PMID: 19667332
-
[Analysis of clinicopathologic characteristics of 422 conjunctival melanocytic nevi specimens].Zhonghua Yan Ke Za Zhi. 2017 Aug 11;53(8):583-587. doi: 10.3760/cma.j.issn.0412-4081.2017.08.005. Zhonghua Yan Ke Za Zhi. 2017. PMID: 28851198 Chinese.
-
Inflammatory juvenile compound conjunctival nevi. A clinicopathological study and literature review.Rom J Morphol Embryol. 2017;58(3):739-747. Rom J Morphol Embryol. 2017. PMID: 29250649 Review.
-
Role of In Vivo Reflectance Confocal Microscopy in the Analysis of Melanocytic Lesions.Acta Dermatovenerol Croat. 2018 Apr;26(1):64-67. Acta Dermatovenerol Croat. 2018. PMID: 29782304 Review.
Cited by
-
Pigmented Conjunctival Nevus: A Mystery Solved by Histopathology.Cureus. 2024 Jul 14;16(7):e64528. doi: 10.7759/cureus.64528. eCollection 2024 Jul. Cureus. 2024. PMID: 39139338 Free PMC article.
References
-
- Zimmerman LE, Sobin LH, editors. World Health Organization (WHO) histological typing of tumours of the eye and its adnexa. International Histological Classification of Tumours No 24. Geneva Switzerland: WHO; 1980. https://apps.who.int/iris/handle/10665/41599
-
- Grossniklaus HE, Eberhart CG, Kivelä TT, editors. World Health Organization (WHO) classification of tumours of the eye. 4. Lyon France: International Agency for Research on Cancer (IARC) Press; 2018. https://publications.iarc.fr/Book-And-Report-Series/Who-Classification-O...
-
- Shields CL, Sioufi K, Alset AE, Boal NS, Casey MG, Knapp AN, Sugarman JA, Schoen MA, Gordon PS, Say EAT, Shields JA. Clinical features differentiating benign from malignant conjunctival tumors in children. JAMA Ophthalmol. 2017;135(3):215–224. - PubMed
-
- Shields CL, Shields JA. Conjunctival tumors in children. Curr Opin Ophthalmol. 2007;18(5):351–360. - PubMed
-
- Rakusiewicz K, Kanigowska K, Grajkowska W, Hautz W. Surgical treatment of conjunctival nevi in pediatric patients. Klinika Oczna (Acta Ophthalmol Pol) 2019;121(1):29–33. http://www.klinikaoczna.pl/Surgical-treatment-of-conjunctival-nevi-in-pe...
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

