Evaluation of the association of anticholinergic burden and delirium in older hospitalised patients - A cohort study comparing 19 anticholinergic burden scales
- PMID: 35675080
- PMCID: PMC9796852
- DOI: 10.1111/bcp.15432
Evaluation of the association of anticholinergic burden and delirium in older hospitalised patients - A cohort study comparing 19 anticholinergic burden scales
Abstract
Aims: A recent review identified 19 anticholinergic burden scales (ABSs) but no study has yet compared the impact of all 19 ABSs on delirium. We evaluated whether a high anticholinergic burden as classified by each ABS is associated with incident delirium.
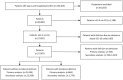
Method: We performed a retrospective cohort study in a Swiss tertiary teaching hospital using data from 2015-2018. Included were patients aged ≥65, hospitalised ≥48 hours with no stay >24 hours in intensive care. Delirium was defined twofold: (i) ICD-10 or CAM and (ii) ICD-10 or CAM or DOSS. Patients' cumulative anticholinergic burden score, calculated within 24 hours after admission, was classified using a binary (<3: low, ≥3: high burden) and a categorical approach (0: no, 0.5-3: low, ≥3: high burden). Association was analysed using multivariable logistic regression.
Results: Over 25 000 patients (mean age 77.9 ± 7.6 years) were included. Of these, (i) 864 (3.3%) and (ii) 2770 (11.0%) developed delirium. Depending on the evaluated ABS, 4-63% of the patients were exposed to at least one anticholinergic drug. Out of 19 ABSs, (i) 14 and (ii) 16 showed a significant association with the outcomes. A patient with a high anticholinergic burden score had odds ratios (ORs) of 1.21 (95% confidence interval [CI]: 1.03-1.42) to 2.63 (95% CI: 2.28-3.03) for incident delirium compared to those with low or no burden.
Conclusion: A high anticholinergic burden within 24 hours after admission was significantly associated with incident delirium. Although prospective studies need to confirm these results, discontinuing or substituting drugs with a score of ≥3 at admission might be a targeted intervention to reduce incident delirium.
Keywords: DOSS; anticholinergic burden; delirium during hospitalisation; older patients.
© 2022 The Authors. British Journal of Clinical Pharmacology published by John Wiley & Sons Ltd on behalf of British Pharmacological Society.
Conflict of interest statement
The authors declare they have no conflicts of interest.
Figures
References
-
- Young J, Inouye SK. Delirium in older people. BMJ. 2007;334(7598):842‐846. doi: 10.1136/bmj.39169.706574.AD - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical