Return to Work of Healthcare Workers after SARS-CoV-2 Infection: Determinants of Physical and Mental Health
- PMID: 35682394
- PMCID: PMC9180816
- DOI: 10.3390/ijerph19116811
Return to Work of Healthcare Workers after SARS-CoV-2 Infection: Determinants of Physical and Mental Health
Abstract
Introduction. The SARS-CoV-2 pandemic has involved healthcare workers (HCWs) both as caregivers and as patients. This study is a retrospective cross-sectional analysis of the HCWs working in a third-level hospital in Central Italy who were infected with COVID-19 from March 2020 to April 2021. This research aims at identifying the physical and mental health outcomes of HCWs infected with COVID-19 who returned to work after the infection, the determinants of those outcomes, such as age and sex, and the identification of possible vulnerable professional groups. Methods. A questionnaire about the acute illness, the experience of returning to work, and health perceptions after the disease was administered to 427 healthcare workers 3 months after recovering from the SARS-CoV-2 infection. Results. The majority interviewed (84.5%) reported symptoms at the time of the positive test, with no significant differences regarding age or sex, while a significant difference in the mean age was found regarding hospitalization (p < 0.001). At 3 months after the infection, females (p = 0.001), older workers (p < 0.001), and healthcare assistants (p < 0.001) were more likely to report persistent symptoms. Sex (p = 0.02) and age (p = 0.006) influenced the quality of sleep after the infection. At work, the nurses group reported increase in workload (p = 0.03) and worse relationships (p = 0.028). At 3 months after the infection, female workers perceived worse physical (p = 0.002) and mental (p < 0.001) health status according to the SF-12. A negative correlation was found between age and PCS score (p < 0.001) but not MCS score (p = 0.86). A significant difference in PCS score was found between nurses and physicians (p = 0.04) and between residents and all other groups (p < 0.001). Finally, the group of workers reporting sleep alterations showed lower PCS and MCS scores (p < 0.001) and working relationships had an impact on MCS scores (p < 0.001). Conclusions. Age, sex, and type of job had an impact on physical and mental outcomes. Organizing specific interventions, also tailored to professional sub-groups, should be a target for healthcare systems to protect and boost the physical and mental health of their workers.
Keywords: SARS-CoV-2 infection; aging workforce; gender; health perception; healthcare workers; occupational health; occupational wellbeing; resilience; return to work; sleep alterations.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

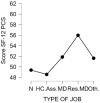
References
-
- Update on Omicron. [(accessed on 3 December 2021)]. Available online: https://www.who.int/news/item/28-11-2021-update-on-omicron.
-
- Gómez-Ochoa S.A., Franco O.H., Rojas L.Z., Raguindin P.F., Roa-Díaz Z.M., Wyssmann B.M., Guevara S.L.R., Echeverría L.E., Glisic M., Muka T. COVID-19 in Health-Care Workers: A Living Systematic Review and Meta-Analysis of Prevalence, Risk Factors, Clinical Characteristics, and Outcomes. Am. J. Epidemiol. 2021;190:161–175. doi: 10.1093/aje/kwaa191. - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

