The Association of Early Corticosteroid Therapy With Clinical and Health-Related Quality of Life Outcomes in Children With Septic Shock
- PMID: 35695852
- PMCID: PMC9444900
- DOI: 10.1097/PCC.0000000000003009
The Association of Early Corticosteroid Therapy With Clinical and Health-Related Quality of Life Outcomes in Children With Septic Shock
Erratum in
-
The Association of Early Corticosteroid Therapy With Clinical and Health-Related Quality of Life Outcomes in Children With Septic Shock: Erratum.Pediatr Crit Care Med. 2023 Apr 1;24(4):e212. doi: 10.1097/PCC.0000000000003204. Epub 2023 Apr 6. Pediatr Crit Care Med. 2023. PMID: 37026731 No abstract available.
Abstract
Objectives: Corticosteroids are commonly used in the treatment of pediatric septic shock without clear evidence of the potential benefits or risks. This study examined the association of early corticosteroid therapy with patient-centered clinically meaningful outcomes.
Design: Subsequent cohort analysis of data derived from the prospective Life After Pediatric Sepsis Evaluation (LAPSE) investigation. Outcomes among patients receiving hydrocortisone or methylprednisolone on study day 0 or 1 were compared with those who did not use a propensity score-weighted analysis that controlled for age, sex, study site, and measures of first-day illness severity.
Setting: Twelve academic PICUs in the United States.
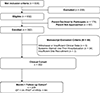
Patients: Children with community-acquired septic shock 1 month to 18 years old enrolled in LAPSE, 2013-2017. Exclusion criteria included a history of chronic corticosteroid administration.
Interventions: None.
Measurements and main results: Among children enrolled in LAPSE, 352 of 392 met analysis inclusion criteria, and 155 of 352 (44%) received early corticosteroid therapy. After weighting corticosteroid therapy administration propensity across potentially confounding baseline characteristics, differences in outcomes associated with treatment were not statistically significant (adjusted effect or odds ratio [95% CI]): vasoactive-inotropic support duration (-0.37 d [-1.47 to 0.72]; p = 0.503), short-term survival without new morbidity (1.37 [0.83-2.28]; p = 0.218), new morbidity among month-1 survivors (0.70 [0.39-1.23]; p = 0.218), and persistent severe deterioration of health-related quality of life or mortality at month 1 (0.70 [0.40-1.23]; p = 0.212).
Conclusions: This study examined the association of early corticosteroid therapy with mortality and morbidity among children encountering septic shock. After adjusting for variables with the potential to confound the relationship between early corticosteroid administration and clinically meaningful end points, there was no improvement in outcomes associated with this therapy. Results from this propensity analysis provide additional justification for equipoise regarding corticosteroid therapy for pediatric septic shock and ascertain the need for a well-designed clinical trial to examine benefit/risk for this intervention.
Copyright © 2022 by the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies.
Conflict of interest statement
Drs. Banks’, Carcillo’s, Sorenson’s, and Zimmerman’s institutions received funding from the National Institute of Child Health and Human Development. Drs. Banks, Reeder, Berg, Newth, Pollack, Meert, Carcillo, Mourani, Sorenson, Varni, Cengiz, and Zimmerman received support for article research from the National Institutes of Health (NIH). Drs. Reeder’s, Berg’s, Newth’s, Pollack’s, Meert’s, Mourani’s, and Varni’s institutions received funding from the NIH. Dr. Newth received funding from Philips Research North America, Hamilton Medical, and Nihon Kohden Orange Med. Dr. Zimmerman’s institution received funding from Immunexpress; he received funding from Elsevier Publishing; he disclosed the off-label product use of Corticosteroids as adjunctive treatment for pediatric septic shock. Dr. Kamps has disclosed that she does not have any potential conflicts of interest.
Figures
Comment in
-
Associations Between Early Corticosteroids, Pediatric Septic Shock, and Outcomes: Not a Simple Analysis.Pediatr Crit Care Med. 2022 Sep 1;23(9):749-751. doi: 10.1097/PCC.0000000000003036. Epub 2022 Aug 29. Pediatr Crit Care Med. 2022. PMID: 36053035 No abstract available.
References
-
- Fleischmann-Struzek C, Goldfarb DM, Schlattmann P, et al. : The global burden of paediatric and neonatal sepsis: a systematic review. Lancet Respir Med 2018; 6:223–230 - PubMed
-
- Glass RI, Guttmacher AE, Black RE: Ending preventable child death in a generation. JAMA - J Am Med Assoc 2012; 308:141–142 - PubMed
-
- Liu L, Johnson HL, Cousens S, et al. : Global, regional, and national causes of child mortality: An updated systematic analysis for 2010 with time trends since 2000. Lancet 2012; 379:2151–2161 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- U10 HD050012/HD/NICHD NIH HHS/United States
- UG1 HD049983/HD/NICHD NIH HHS/United States
- UG1 HD050096/HD/NICHD NIH HHS/United States
- U10 HD063106/HD/NICHD NIH HHS/United States
- UG1 HD063108/HD/NICHD NIH HHS/United States
- R01 HD073362/HD/NICHD NIH HHS/United States
- UG1 HD083171/HD/NICHD NIH HHS/United States
- U01 HD049934/HD/NICHD NIH HHS/United States
- UG1 HD083170/HD/NICHD NIH HHS/United States
- UG1 HD083166/HD/NICHD NIH HHS/United States
- PL1 HD105462/HD/NICHD NIH HHS/United States
- UG1 HD049981/HD/NICHD NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

