[Effects of gestational weight on the association between serum high sensitivity C reaction protein and gestational diabetes mellitus among twin gestations: A cohort study]
- PMID: 35701118
- PMCID: PMC9197712
- DOI: 10.19723/j.issn.1671-167X.2022.03.006
[Effects of gestational weight on the association between serum high sensitivity C reaction protein and gestational diabetes mellitus among twin gestations: A cohort study]
Abstract
Objective: To investigate the association between serum high sensitivity C-reaction protein (hsCRP) in early pregnancy and gestational diabetes mellitus (GDM) among twin pregnant women, and to explore the effects of the pre-pregnant body mass index (BMI) and gestational weight gain (GWG) status on such association.
Methods: Twin pregnant women with pre-pregnant BMI greater than or equal to 18.5 kg/m2 were recruited at Department of Obstetrics and Gynecology of Peking University Third Hospital from March 2017 to December 2020. Serum samples collected in early pregnancy were analyzed for hsCRP using particle-enhanced immunoturbidimetric method. In the following visits, the information about GWG and GDM were prospectively collected in every trimester. The association effect between hsCRP tertiles and GDM were estimated using Logistic regression, and further converted into risk ratio (RR). Cochran-Mantel-Haenszel test and mediation analysis were used to explore the effects of BMI and GWG status on the association.
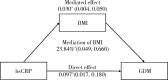
Results: Among the included 570 twin pregnant women, 31.6% deve-loped GDM, 26.1% were pre-pregnant overweight or obesity, and 49.5% with GWG out of referenced range. After adjustment for confounding factors, risk of developing GDM in twin gestations with the middle tertile and highest tertile of serum hsCRP in early pregnancy were 1.42 fold (95%CI: 1.02-1.89) and 1.54 fold (95%CI: 1.12-2.02), respectively, compared with the lowest tertile of serum hsCRP, and there existed significantly linear trend (P=0.022). Findings from mediation analysis illustrated that pre-pregnant BMI had partial mediating effect on the association, and BMI accounted for 23.84% (P < 0.001) of the increasing GDM risks with elevated hsCRP. Joint analysis with hsCRP and GWG found that those who were with GWG out of referenced range accompanied with the higher hsCRP tertiles (>1.21 mg/L) had significantly 2.31 fold increased risk according to those who were with GWG in the referenced range accompanied with the lowest hsCRP tertile (≤1.21 mg/L, P < 0.01).
Conclusion: Elevated hsCRP in early pregnancy significantly increased GDM risk among twin pregnant women. The hsCRP-GDM association was dependent on GWG status, and pre-pregnant BMI had partial mediating effect on such association. It is suggested that twin pregnant women should consider systemic inflammation and gestational weight at the same time to reduce GDM risk.
目的: 探讨双胎妊娠孕妇孕早期血清高敏C反应蛋白(high sensitivity C-reaction protein,hsCRP)与妊娠期糖尿病(gestational diabetes mellitus, GDM)的关联,以及孕前体重指数(body mass index,BMI)和孕期增重情况对这一关联的影响。
方法: 选取2017年3月至2020年12月在北京大学第三医院产科募集的孕前BMI ≥18.5 kg/m2的双胎孕妇,采用颗粒增强免疫透射比浊法检测孕早期血清hsCRP,前瞻性随访得到孕期增重和GDM的发生情况。采用Logistic回归分析hsCRP与GDM的关联效应,转换得到风险比(risk ratio, RR),采用分层卡方检验、中介效应分析BMI、孕期增重情况对hsCRP与GDM关联的影响。
结果: 570名双胎妊娠孕妇中,31.6%发生了GDM,26.1%孕前超重或肥胖,49.5%孕期增重超过推荐范围。调整混杂因素后,孕早期血清hsCRP中三分位和上三分位发生GDM的风险是下三分位的1.42倍(95%CI:1.02~1.89)和1.54倍(95%CI:1.12~2.02),且呈线性趋势(P=0.022)。中介效应分析表明,孕前BMI对高水平hsCRP增加GDM风险的解释程度为23.84% (P < 0.001),对两者的关联存在部分中介效应。联合hsCRP和孕期增重情况发现,孕期增重超过推荐范围且hsCRP较高水平(>1.21 mg/L)者发生GDM的风险是孕期增重在推荐范围内且hsCRP在下三分位者的2.31倍(P < 0.01)。
结论: 孕早期高水平hsCRP显著增加双胎妊娠发生GDM的风险,hsCRP-GDM关联独立于孕期增重,且孕前BMI对hsCRP-GDM关联存在部分中介效应。双胎妊娠孕期管理要同时注重全身炎症反应和孕期体质量,以降低GDM发生风险。
Keywords: Body mass index; C-reactive protein; Diabetes, gestational; Twin pregnancy.
Figures
Similar articles
-
Late-pregnancy dysglycemia in obese pregnancies after negative testing for gestational diabetes and risk of future childhood overweight: An interim analysis from a longitudinal mother-child cohort study.PLoS Med. 2018 Oct 29;15(10):e1002681. doi: 10.1371/journal.pmed.1002681. eCollection 2018 Oct. PLoS Med. 2018. PMID: 30372451 Free PMC article.
-
Pre-pregnancy body mass index, gestational diabetes mellitus, and gestational weight gain: individual and combined effects on fetal growth.Front Public Health. 2024 Mar 11;12:1354355. doi: 10.3389/fpubh.2024.1354355. eCollection 2024. Front Public Health. 2024. PMID: 38528861 Free PMC article.
-
Correlation of body composition in early pregnancy on gestational diabetes mellitus under different body weights before pregnancy.Front Endocrinol (Lausanne). 2022 Oct 28;13:916883. doi: 10.3389/fendo.2022.916883. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 36387861 Free PMC article.
-
[Maternal and neonatal outcomes according to gestational weight gain in twin pregnancies: Are the IOM guidelines associated with better issues?].Gynecol Obstet Fertil Senol. 2017 Jun;45(6):366-372. doi: 10.1016/j.gofs.2017.02.003. Epub 2017 Mar 31. Gynecol Obstet Fertil Senol. 2017. PMID: 28366706 Review. French.
-
Gestational Metabolic Risk: A Narrative Review of Pregnancy-Related Complications and of the Effectiveness of Dietary, Exercise and Lifestyle Interventions during Pregnancy on Reducing Gestational Weight Gain and Preventing Gestational Diabetes Mellitus.J Clin Med. 2024 Jun 13;13(12):3462. doi: 10.3390/jcm13123462. J Clin Med. 2024. PMID: 38929991 Free PMC article. Review.
References
-
- American Diabetes Association 14. Management of diabetes in pregnancy: Standards of Medical Care in Diabetes-2021. Diabetes Care. 2021;44(Suppl 1):S200–S210. - PubMed
-
- Hiersch L, Berger H, Okby R, et al. Gestational diabetes mellitus is associated with adverse outcomes in twin pregnancies. Am J Obstet Gynecol. 2019;220(1):101–102. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials