Longitudinal evaluation of neurologic-post acute sequelae SARS-CoV-2 infection symptoms
- PMID: 35702954
- PMCID: PMC9268882
- DOI: 10.1002/acn3.51578
Longitudinal evaluation of neurologic-post acute sequelae SARS-CoV-2 infection symptoms
Abstract
Objective: To assess the initial features and evolution of neurologic Postacute Sequelae of SARS-CoV-2 infection (neuro-PASC) in patients with and without prior neurologic disease.
Methods: Participants with neurologic symptoms following acute SARS-CoV-2 infection were recruited from October 9, 2020 to October 11, 2021. Clinical data included a SARS-CoV-2 infection history, neurologic review of systems, neurologic exam, Montreal cognitive assessment (MoCA), and symptom-based self-reported surveys at baseline (conducted after acute infection) and 6-month follow-up assessments.
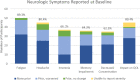
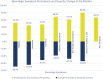
Results: Fifty-six participants (69% female, mean age 50 years, 29% with prior neurologic disease such as multiple sclerosis) were enrolled, of which 27 had completed the 6-month follow-up visit in this ongoing study. SARS-CoV-2 infection severity was largely described as mild (39.3%) or moderate (42.9%). At baseline, following acute infection, the most common neurologic symptoms were fatigue (89.3%) and headaches (80.4%). At the 6-month follow-up, memory impairment (68.8%) and decreased concentration (61.5%) were the most prevalent, though on average all symptoms showed a reduction in reported severity score at the follow-up. Complete symptom resolution was reported in 33.3% of participants by 6 months. From baseline to 6 months, average MoCA scores improved overall though 26.3% of participants' scores decreased. A syndrome consisting of tremor, ataxia, and cognitive dysfunction (PASC-TAC) was observed in 7.1% of patients.
Interpretation: Early in the neuro-PASC syndrome, fatigue and headache are the most commonly reported symptoms. At 6 months, memory impairment and decreased concentration were most prominent. Only one-third of participants had completed resolution of neuro-PASC at 6 months, although persistent symptoms trended toward improvement at follow-up.
Keywords: COVID-19; postacute sequelae of COVID-19 infection.
© 2022 The Authors. Annals of Clinical and Translational Neurology published by Wiley Periodicals LLC on behalf of American Neurological Association.
Conflict of interest statement
Jacqueline Shanley, Andrew Valenciano, Garrett Timmons, Visesha Kakarla, Annalise Miner, Amanda Gooding, Lucy Horton, Ronald Ellis, Marc Norman, and Torge Rempe do not have anything to disclose. Unrelated to this manuscript, Jennifer Yang has participated in a sponsored talk, Neurology Live MS Medications 2021. Unrelated to the current work, Sarah Banks have consulted with Boston University on NINDS funded grant and participated in the data safety monitoring board for Cleveland Clinic Foundation (NIA funded RO1). Last, unrelated to the current work, Jennifer Graves over the past year has grant/contract research support from the National MS Society, Biogen, and Octave Biosciences. She serves on a steering committee for a trial supported by Novartis. She has received honoraria for a nonpromotional, educational activity for Sanofi‐Genzyme. She has received speaker fees from Alexion and BMS and served on an advisory board for Genentech.
Figures
References
-
- Collins F. NIH Director's Blog. “Post‐Acute Sequelae of COVID‐19.” Accessed December 11, 2021. https://directorsblog.nih.gov/tag/post‐acute‐sequelae‐of‐covid‐19/
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
