Prevention of lymphocele or seroma after mastectomy and axillary lymphadenectomy for breast cancer: systematic review and meta-analysis
- PMID: 35705655
- PMCID: PMC9200791
- DOI: 10.1038/s41598-022-13831-9
Prevention of lymphocele or seroma after mastectomy and axillary lymphadenectomy for breast cancer: systematic review and meta-analysis
Abstract
Seroma or lymphocele remains the most common complication after mastectomy and lymphadenectomy for breast cancer. Many different techniques are available to prevent this complication: wound drainage, reduction of the dead space by flap fixation, use of various types of energy, external compression dressings, shoulder immobilization or physical activity, as well as numerous drugs and glues. We searched MEDLINE, clinicaltrials.gov, Cochrane Library, and Web of Science databases for publications addressing the issue of prevention of lymphocele or seroma after mastectomy and axillary lymphadenectomy. Quality was assessed using Hawker's quality assessment tool. Incidence of seroma or lymphocele were collected. Fifteen randomized controlled trials including a total of 1766 patients undergoing radical mastectomy and axillary lymphadenectomy for breast cancer were retrieved. The incidence of lymphocele or seroma in the study population was 24.2% (411/1698): 25.2% (232/920) in the test groups and 23.0% (179/778) in the control groups. Neither modification of surgical technique (RR 0.86; 95% CI [0.72, 1.03]) nor application of a medical treatment (RR 0.96; 95% CI [0.72, 1.29]) was effective in preventing lymphocele. On the contrary, decreasing the drainage time increased the risk of lymphocele (RR 1.88; 95% CI [1.43, 2.48). There was no publication bias but the studies were of medium to low quality. To conclude, despite the heterogeneity of study designs, drainage appears to be the most effective technique, although the overall quality of the data is low.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures


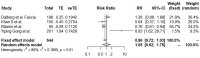

Similar articles
-
OK-432 (Sapylin) Reduces Seroma Formation After Axillary Lymphadenectomy in Breast Cancer.J Invest Surg. 2017 Feb;30(1):1-5. doi: 10.1080/08941939.2016.1204386. Epub 2016 Jul 18. J Invest Surg. 2017. PMID: 27431576 Clinical Trial.
-
Flap fixation in preventing seroma formation after mastectomy: an updated meta-analysis.Updates Surg. 2021 Aug;73(4):1307-1314. doi: 10.1007/s13304-021-01049-9. Epub 2021 Apr 22. Updates Surg. 2021. PMID: 33886107 Free PMC article. Review.
-
A single-center, randomized, non-inferiority study evaluating seroma formation after mastectomy combined with flap fixation with or without suction drainage: protocol for the Seroma reduction and drAin fRee mAstectomy (SARA) trial.BMC Cancer. 2020 Aug 7;20(1):735. doi: 10.1186/s12885-020-07242-0. BMC Cancer. 2020. PMID: 32767988 Free PMC article.
-
[Quilting suture after mastectomy in prevention of postoperative seroma: a prospective observational study].Gynecol Obstet Fertil. 2015 Mar;43(3):205-12. doi: 10.1016/j.gyobfe.2015.01.007. Epub 2015 Feb 21. Gynecol Obstet Fertil. 2015. PMID: 25708845 French.
-
[Seroma after axillary lymph node dissection in breast cancer].Gynecol Obstet Fertil. 2008 Feb;36(2):130-135. doi: 10.1016/j.gyobfe.2007.07.040. Gynecol Obstet Fertil. 2008. PMID: 18243754 Review. French.
Cited by
-
Monopolar diathermy versus a vessel-sealing device for reducing postoperative drain output after simple mastectomy: randomized clinical trial.Br J Surg. 2024 Mar 2;111(3):znae029. doi: 10.1093/bjs/znae029. Br J Surg. 2024. PMID: 38498075 Free PMC article. Clinical Trial.
-
The Efficacy and Safety of Somatostatin Analog after Axillary Node Dissection in Breast Cancer: A Systematic Review and Meta-analysis.JMA J. 2023 Jul 14;6(3):274-281. doi: 10.31662/jmaj.2022-0219. Epub 2023 May 22. JMA J. 2023. PMID: 37560373 Free PMC article. Review.
-
Comparison of the effect of ultrasounic-harmonic scalpel and electrocautery in the treatment of axillary lymph nodes during radical surgery for breast cancer.World J Surg Oncol. 2024 Apr 11;22(1):91. doi: 10.1186/s12957-024-03381-x. World J Surg Oncol. 2024. PMID: 38600546 Free PMC article.
-
Postoperative lymphatic leakage following laparoscopic totally extraperitoneal inguinal hernia repair: the first case report and review of the literature.Hernia. 2025 Mar 27;29(1):126. doi: 10.1007/s10029-025-03318-7. Hernia. 2025. PMID: 40146374 Review.
-
The Effects of Systemic Tranexamic Acid Administration on Drainage Volume, Duration of Drain Placement, and Length of Hospital Stay in Skin- and Nipple-Sparing Mastectomies with Immediate Expander-Based Breast Reconstruction.J Clin Med. 2024 Oct 30;13(21):6507. doi: 10.3390/jcm13216507. J Clin Med. 2024. PMID: 39518646 Free PMC article.
References
-
- Lucci A, McCall LM, Beitsch PD, Whitworth PW, Reintgen DS, Blumencranz PW, Leitch AM, Saha S, Hunt KK, Giuliano AE, American College of Surgeons Oncology Group Surgical complications associated with sentinel lymph node dissection (SLND) plus axillary lymph node dissection compared with SLND alone in the American College of Surgeons Oncology Group Trial Z0011. J. Clin. Oncol. 2007;25(24):3657–3663. doi: 10.1200/JCO.2006.07.4062. - DOI - PubMed
-
- Granzier RWY, van Bastelaar J, van Kuijk SMJ, Hintzen KFH, Heymans C, Theunissen LLB, et al. Reducing seroma formation and its sequelae after mastectomy by closure of the dead space: The interim analysis of a multi-center, double-blind randomized controlled trial (SAM trial) Breast. 2019;46:81–86. doi: 10.1016/j.breast.2019.05.002. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

