Hepatitis C Co-infection in People Living With HIV-Epidemiologic Differences Between Men Who Have Sex With Men MSM and Non-MSM
- PMID: 35719672
- PMCID: PMC9204175
- DOI: 10.3389/fpubh.2022.925600
Hepatitis C Co-infection in People Living With HIV-Epidemiologic Differences Between Men Who Have Sex With Men MSM and Non-MSM
Abstract
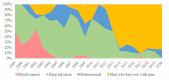
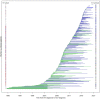
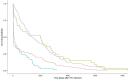
People living with human immunodeficiency virus (PLHIV) constitute a unique group at higher risk of hepatitis C virus (HCV) co-infection. In light of the diverse profiles of PLHIV, we differentiated between men who have sex with men (MSM) and non-MSM in the characterization of the epidemiologic features of HIV/HCV co-infection. Clinical data of HCV co-infection patients from the HIV specialist clinic in Hong Kong were retrospectively collected in conjunction with their HIV subtypes and HCV genotypes. Logistic regression models were used to identify factors associated with HIV/HCV co-infection in MSM. Survival analysis was performed to compare the time lag between HIV and HCV diagnoses between two groups. Latent class analysis was conducted to describe the features of different classes of co-infections. Four classes of HIV/HCV co-infections were identified: local MSM acquiring HCV after HIV diagnosis, local MSM with HIV/HCV co-diagnoses, local non-MSM, and non-local non-MSM. Accounting for over half of the co-infections, MSM were more likely to be younger, local residents, and associated with HCV genotype 3, compared to genotypes 1 and 6 in non-MSM. Overall, MSM had higher odds of achieving HIV viral suppression and co-diagnosing with a sexually transmitted infection at HCV diagnosis, and having a longer time lag between HIV and HCV diagnoses. Drug injection accounted for a majority of non-MSM HCV infection. There were distinctive epidemiologic differences between MSM and non-MSM co-infected with HIV and HCV, the characteristics of which could inform intervention strategies for achieving HCV micro-elimination.
Keywords: HIV/HCV co-infection; men who have sex with men; molecular epidemiology; people living with HIV; people who inject drugs.
Copyright © 2022 Kwan, Wong, Wong and Lee.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Diverse origins of hepatitis C virus in HIV co-infected men who have sex with men in Hong Kong.Virol J. 2015 Aug 8;12:120. doi: 10.1186/s12985-015-0355-8. Virol J. 2015. PMID: 26253209 Free PMC article.
-
A latent class approach to identify multi-risk profiles associated with phylogenetic clustering of recent hepatitis C virus infection in Australia and New Zealand from 2004 to 2015.J Int AIDS Soc. 2019 Feb;22(2):e25222. doi: 10.1002/jia2.25222. J Int AIDS Soc. 2019. PMID: 30746864 Free PMC article.
-
Risk factors associated with HCV co-infection amongst MSM and transgender women living with HIV in Mexico City: A case-control study.Ann Hepatol. 2022 Nov-Dec;27(6):100758. doi: 10.1016/j.aohep.2022.100758. Epub 2022 Sep 10. Ann Hepatol. 2022. PMID: 36096295
-
Sexually transmitted hepatitis C virus infections: current trends, and recent advances in understanding the spread in men who have sex with men.J Int AIDS Soc. 2019 Aug;22 Suppl 6(Suppl Suppl 6):e25348. doi: 10.1002/jia2.25348. J Int AIDS Soc. 2019. PMID: 31468692 Free PMC article.
-
Risk of hepatitis C reinfection following successful therapy among people living with HIV: a global systematic review, meta-analysis, and meta-regression.Lancet HIV. 2022 Jun;9(6):e414-e427. doi: 10.1016/S2352-3018(22)00077-7. Lancet HIV. 2022. PMID: 35659336
References
-
- World Health Organization. Global Hepatitis Report, 2017 . (2017). Available online at: https://www.who.int/publications/i/item/global-hepatitis-report-2017 (accessed December 1, 2021).
-
- World Health Organization. Hepatitis C. (2021). Available online at: https://www.who.int/news-room/fact-sheets/detail/hepatitis-c (accessed December 1, 2021).
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

