Polypharmacy, comorbidity and frailty: a complex interplay in older patients at the emergency department
- PMID: 35723840
- PMCID: PMC9378326
- DOI: 10.1007/s41999-022-00664-y
Polypharmacy, comorbidity and frailty: a complex interplay in older patients at the emergency department
Abstract
Purpose: Older adults at the emergency department (ED) with polypharmacy, comorbidity, and frailty are at risk of adverse health outcomes. We investigated the association of polypharmacy with adverse health outcomes, in relation to comorbidity and frailty.
Methods: This is a prospective cohort study in ED patients ≥ 70 years. Non-polypharmacy was defined as 0-4 medications, polypharmacy 5-9 and excessive polypharmacy ≥ 10. Comorbidity was classified by the Charlson comorbidity index (CCI). Frailty was defined by the Identification of Seniors At Risk-Hospitalized Patients (ISAR-HP) score. The primary outcome was 3-month mortality. Secondary outcomes were readmission to an ED/hospital ward and a self-reported fall < 3 months. The association between polypharmacy, comorbidity and frailty was analyzed by logistic regression.
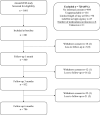
Results: 881 patients were included. 43% had polypharmacy and 18% had excessive polypharmacy. After 3 months, 9% died, 30% were readmitted, and 21% reported a fall. Compared with non-polypharmacy, the odds ratio (OR) for mortality ranged from 2.62 (95% CI 1.39-4.93) in patients with polypharmacy to 3.92 (95% CI 1.95-7.90) in excessive polypharmacy. The OR weakened after adjustment for comorbidity: 1.80 (95% CI 0.92-3.52) and 2.32 (95% CI 1.10-4.90). After adjusting for frailty, the OR weakened to 2.10 (95% CI 1.10-4.00) and OR 2.40 (95% CI 1.15-5.02). No significant association was found for readmission or self-reported fall.
Conclusions: Polypharmacy is common in older patients at the ED. Polypharmacy, and especially excessive polypharmacy, is associated with an increased risk of mortality. The observed association is complex given the confounding effect of comorbidity and frailty.
Keywords: Comorbidity; Emergency department; Frailty; Older adults; Polypharmacy.
© 2022. The Author(s).
Conflict of interest statement
The authors have no relevant financial or non-financial interests to disclose.
Figures

References
-
- Lemmens LC, Weda M (2013) Improving medication safety for the elderly; some bottlenecks (no. 0880027001/2013). RIVM brief rapport. https://www.rivm.nl/bibliotheek/rapporten/080027001.pdf. Accessed April 1, 2022
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
