Driving pressure-guided ventilation decreases the mechanical power compared to predicted body weight-guided ventilation in the Acute Respiratory Distress Syndrome
- PMID: 35725498
- PMCID: PMC9208543
- DOI: 10.1186/s13054-022-04054-5
Driving pressure-guided ventilation decreases the mechanical power compared to predicted body weight-guided ventilation in the Acute Respiratory Distress Syndrome
Abstract
Background: Whether targeting the driving pressure (∆P) when adjusting the tidal volume in mechanically ventilated patients with the acute respiratory distress syndrome (ARDS) may decrease the risk of ventilator-induced lung injury remains a matter of research. In this study, we assessed the effect of a ∆P-guided ventilation on the mechanical power.
Methods: We prospectively included adult patients with moderate-to-severe ARDS. Positive end expiratory pressure was set by the attending physician and kept constant during the study. Tidal volume was first adjusted to target 6 ml/kg of predicted body weight (PBW-guided ventilation) and subsequently modified within a range from 4 to 10 ml/kg PBW to target a ∆P between 12 and 14 cm H2O. The respiratory rate was then re-adjusted within a range from 12 to 40 breaths/min until EtCO2 returned to its baseline value (∆P-guided ventilation). Mechanical power was computed at each step.
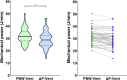
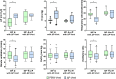
Results: Fifty-one patients were included between December 2019 and May 2021. ∆P-guided ventilation was feasible in all but one patient. The ∆P during PBW-guided ventilation was already within the target range of ∆P-guided ventilation in five (10%) patients, above in nine (18%) and below in 36 (72%). The change from PBW- to ∆P-guided ventilation was thus accompanied by an overall increase in tidal volume from 6.1 mL/kg PBW [5.9-6.2] to 7.7 ml/kg PBW [6.2-8.7], while respiratory rate was decreased from 29 breaths/min [26-32] to 21 breaths/min [16-28] (p < 0.001 for all comparisons). ∆P-guided ventilation was accompanied by a significant decrease in mechanical power from 31.5 J/min [28-35.7] to 28.8 J/min [24.6-32.6] (p < 0.001), representing a relative decrease of 7% [0-16]. With ∆P-guided ventilation, the PaO2/FiO2 ratio increased and the ventilatory ratio decreased.
Conclusion: As compared to a conventional PBW-guided ventilation, a ∆P-guided ventilation strategy targeting a ∆P between 12 and 14 cm H2O required to change the tidal volume in 90% of the patients. Such ∆P-guided ventilation significantly reduced the mechanical power. Whether this physiological observation could be associated with clinical benefit should be assessed in clinical trials.
Keywords: Acute respiratory distress syndrome; Driving pressure; Mechanical power; Mechanical ventilation; Protective ventilation; Tidal volume; Ventilator-induced lung injury.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
Similar articles
-
Mechanical power of ventilation and driving pressure: two undervalued parameters for pre extracorporeal membrane oxygenation ventilation and during daily management?Crit Care. 2023 Mar 14;27(1):111. doi: 10.1186/s13054-023-04375-z. Crit Care. 2023. PMID: 36915183 Free PMC article. Review.
-
Driving Pressure-limited Strategy for Patients with Acute Respiratory Distress Syndrome. A Pilot Randomized Clinical Trial.Ann Am Thorac Soc. 2020 May;17(5):596-604. doi: 10.1513/AnnalsATS.201907-506OC. Ann Am Thorac Soc. 2020. PMID: 32069068 Clinical Trial.
-
End-Expiratory Lung Volume in Patients with Acute Respiratory Distress Syndrome: A Time Course Analysis.Lung. 2016 Aug;194(4):527-34. doi: 10.1007/s00408-016-9892-1. Epub 2016 May 12. Lung. 2016. PMID: 27169535
-
[Analysis of compliance with lung protective mechanical ventilation strategy in patients with acute respiratory distress syndrome].Zhonghua Jie He He Hu Xi Za Zhi. 2024 May 12;47(5):419-429. doi: 10.3760/cma.j.cn112147-20230808-00054. Zhonghua Jie He He Hu Xi Za Zhi. 2024. PMID: 38706063 Chinese.
-
Association between tidal volume size, duration of ventilation, and sedation needs in patients without acute respiratory distress syndrome: an individual patient data meta-analysis.Intensive Care Med. 2014 Jul;40(7):950-7. doi: 10.1007/s00134-014-3318-4. Epub 2014 May 9. Intensive Care Med. 2014. PMID: 24811940 Review.
Cited by
-
Flow-controlled ventilation decreases mechanical power in postoperative ICU patients.Intensive Care Med Exp. 2024 Mar 19;12(1):30. doi: 10.1186/s40635-024-00616-9. Intensive Care Med Exp. 2024. PMID: 38502268 Free PMC article.
-
The Impact of Mechanical Energy Assessment on Mechanical Ventilation: A Comprehensive Review and Practical Application.Med Sci Monit. 2023 Sep 5;29:e941287. doi: 10.12659/MSM.941287. Med Sci Monit. 2023. PMID: 37669252 Free PMC article. Review.
-
Expert perspectives on ECCO2R for acute hypoxemic respiratory failure: consensus of a 2022 European roundtable meeting.Ann Intensive Care. 2024 Aug 22;14(1):132. doi: 10.1186/s13613-024-01353-8. Ann Intensive Care. 2024. PMID: 39174831 Free PMC article.
-
Mechanical power of ventilation and driving pressure: two undervalued parameters for pre extracorporeal membrane oxygenation ventilation and during daily management?Crit Care. 2023 Mar 14;27(1):111. doi: 10.1186/s13054-023-04375-z. Crit Care. 2023. PMID: 36915183 Free PMC article. Review.
-
Comparing the impact of targeting limited driving pressure to low tidal volume ventilation on mortality in mechanically ventilated adults with COVID-19 ARDS: an exploratory target trial emulation.BMJ Open Respir Res. 2024 Oct 1;11(1):e002439. doi: 10.1136/bmjresp-2024-002439. BMJ Open Respir Res. 2024. PMID: 39353713 Free PMC article.
References
-
- Acute Respiratory Distress Syndrome Network. Brower RG, Matthay MA, Morris A, Schoenfeld D, Thompson BT, et al. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. 2000;342(18):1301–1308. doi: 10.1056/NEJM200005043421801. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials

