Persistent Dissociation and Its Neural Correlates in Predicting Outcomes After Trauma Exposure
- PMID: 35730162
- PMCID: PMC9444876
- DOI: 10.1176/appi.ajp.21090911
Persistent Dissociation and Its Neural Correlates in Predicting Outcomes After Trauma Exposure
Erratum in
-
Correction to Lebois et al.Am J Psychiatry. 2022 Aug;179(8):585. doi: 10.1176/appi.ajp.21090911correction. Am J Psychiatry. 2022. PMID: 35921397 No abstract available.
Abstract
Objective: Dissociation, a disruption or discontinuity in psychological functioning, is often linked with worse psychiatric symptoms; however, the prognostic value of dissociation after trauma is inconsistent. Determining whether trauma-related dissociation is uniquely predictive of later outcomes would enable early identification of at-risk trauma populations. The authors conducted the largest prospective longitudinal biomarker study of persistent dissociation to date to determine its predictive capacity for adverse psychiatric outcomes following acute trauma.
Methods: All data were part of the Freeze 2 data release from the Advancing Understanding of Recovery After Trauma (AURORA) study. Study participants provided self-report data about persistent derealization (N=1,464), a severe type of dissociation, and completed a functional MRI emotion reactivity task and resting-state scan 2 weeks posttrauma (N=145). Three-month follow-up reports were collected of posttraumatic stress, depression, pain, anxiety symptoms, and functional impairment.
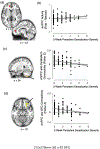
Results: Derealization was associated with increased ventromedial prefrontal cortex (vmPFC) activation in the emotion reactivity task and decreased resting-state vmPFC connectivity with the cerebellum and orbitofrontal cortex. In separate analyses, brain-based and self-report measures of persistent derealization at 2 weeks predicted worse 3-month posttraumatic stress symptoms, distinct from the effects of childhood maltreatment history and current posttraumatic stress symptoms.
Conclusions: The findings suggest that persistent derealization is both an early psychological and biological marker of worse later psychiatric outcomes. The neural correlates of trauma-related dissociation may serve as potential targets for treatment engagement to prevent posttraumatic stress disorder. These results underscore dissociation assessment as crucial following trauma exposure to identify at-risk individuals, and they highlight an unmet clinical need for tailored early interventions.
Keywords: Biological Markers; Depersonalization/Derealization; Dissociative Disorders; Neuroimaging; Posttraumatic Stress Disorder (PTSD).
Conflict of interest statement
Competing Interests Statement:
LAML reports unpaid membership on the Scientific Committee for the International Society for the Study of Trauma and Dissociation (ISSTD), grant support from the National Institute of Mental Health, K01 MH118467, and spousal IP payments from Vanderbilt University for technology licensed to Acadia Pharmaceuticals unrelated to the present work. ISSTD and NIMH were not involved in the analysis or preparation of the manuscript. NGH reports grant support from the National Institute of Mental Health, K00 MH119603. In the last three years GDC has received research funding from the NSF, NIH and LifeBell AI, and unrestricted donations from AliveCor, Amazon Research, the Center for Discovery, the Gordon and Betty Moore Foundation, MathWorks, Microsoft Research, the Gates Foundation, Google, One Mind Foundation, and Samsung Research. GDC has financial interest in AliveCor and receives unrestricted funding from the company. He also is the CTO of MindChild Medical and CSO of LifeBell AI and has ownership in both companies. These relationships are unconnected to the current work. LTG receives an honorarium as a member of the Scientific Advisory Board for Sage Bionetworks as well as funding from the NIH. SLR reports grants from NIH during the conduct of the study; personal fees from SOBP (Society of Biological Psychiatry) paid role as secretary, other from Oxford University Press royalties, other from APP (American Psychiatric Publishing Inc.) royalties, other from VA (Veterans Administration) per diem for oversight committee, and other from Community Psychiatry paid board service, including equity outside the submitted work; and Leadership roles on Board or Council for SOBP, ADAA (Anxiety and Depression Association of America), and NNDC (National Network of Depression Centers). SS has received funding from the Florida Medical Malpractice Joint Underwriter’s Association Dr. Alvin E. Smith Safety of Healthcare Services Grant; Allergan Foundation; the NIH/NIA-funded Jacksonville Aging Studies Center (JAX-ASCENT; R33AG05654); and the Substance Abuse and Mental Health Services Administration (1H79TI083101–01); and the Florida Blue Foundation. CWJ reports no direct conflicts related to this paper. He has been an investigator on studies funded by Hologic Inc, Janssen, AstraZeneca, and Vapotherm, for which his department has received research funding. JJ receives consulting payments from Janssen Pharmaceuticals. Over the past 3 years, DAP has received consulting fees from BlackThorn Therapeutics, Boehringer Ingelheim, Compass Pathway, Concert Pharmaceuticals, Engrail Therapeutics, Otsuka Pharmaceuticals, and Takeda Pharmaceuticals; one honorarium from Alkermes, and research funding from NIMH, Dana Foundation, Brain and Behavior Research Foundation, and Millennium Pharmaceuticals. In addition, he has received stock options from BlackThorn Therapeutics. JWS is PI of a collaborative study of the genetics of depression and bipolar disorder sponsored by 23andMe for which 23andMe provides analysis time as in-kind support but no payments. JME reports support from the National Institutes of Health (NIH) through Grant Numbers R01HD079076 & R03HD094577: Eunice Kennedy Shriver National Institute of Child Health & Human Development; National Center for Medical Rehabilitation Research. He also reports funding from and New South Wales Health, Spinal Cord Injury Award (2020–2025) and consulting fees (< $15,000 per annum) from Orofacial Therapeutics, LLC. In the past 3 years, RCK was a consultant for Datastat, Inc., Holmusk, RallyPoint Networks, Inc., and Sage Pharmaceuticals. He has stock options in Mirah, PYM, and Roga Sciences. All other authors have no conflicts of interest to disclose. KJR serves on advisory boards or has performed scientific consultation for Takeda, Janssen, Bioxcel and Verily, and he has received sponsored research support from Takeda, Alkermes, Alto Neuroscience, and Brainsway. He receives funding from NIH and the Brain and Behavior Research Fund.
Figures
Comment in
-
Looking Through a Fog: What Persistent Derealization Can Teach Us About PTSD.Am J Psychiatry. 2022 Sep;179(9):599-600. doi: 10.1176/appi.ajp.20220573. Am J Psychiatry. 2022. PMID: 36048492 No abstract available.
-
Acute Stress, Traumatic Brain Injury, and Dissociation.Am J Psychiatry. 2023 Apr 1;180(4):318. doi: 10.1176/appi.ajp.20220834. Am J Psychiatry. 2023. PMID: 37002693 No abstract available.
-
Acute Stress, Traumatic Brain Injury, and Dissociation: Response to Simeon.Am J Psychiatry. 2023 Apr 1;180(4):318-319. doi: 10.1176/appi.ajp.20220834r. Am J Psychiatry. 2023. PMID: 37002696 Free PMC article. No abstract available.
References
-
- Spiegel D, Loewenstein RJ, Lewis-Fernández R, et al. : Dissociative disorders in DSM-5. Depress Anxiety 2011; 28:824–852 - PubMed
-
- Sar V, Alioğlu F, Akyuz G: Depersonalization and derealization in self-report and clinical interview: The spectrum of borderline personality disorder, dissociative disorders, and healthy controls. J Trauma Dissociation 2017; 18:490–506 - PubMed
-
- American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders (DSM-5®) American Psychiatric Pub, 2013
-
- Putnam FW: Pierre Janet and modern views of dissociation. J Trauma Stress 1989; 2:413–429

