Application of 68Ga-citrate PET/CT for differentiating periprosthetic joint infection from aseptic loosening after joint replacement surgery
- PMID: 35731211
- PMCID: PMC9233412
- DOI: 10.1302/2046-3758.116.BJR-2021-0464.R1
Application of 68Ga-citrate PET/CT for differentiating periprosthetic joint infection from aseptic loosening after joint replacement surgery
Abstract
Aims: We aimed to evaluate the utility of 68Ga-citrate positron emission tomography (PET)/CT in the differentiation of periprosthetic joint infection (PJI) and aseptic loosening (AL), and compare it with 99mTc-methylene bisphosphonates (99mTc-MDP) bone scan.
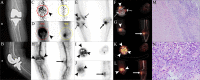
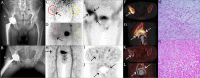
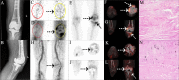
Methods: We studied 39 patients with suspected PJI or AL. These patients underwent 68Ga-citrate PET/CT, 99mTc-MDP three-phase bone scan and single-photon emission CT (SPECT)/CT. PET/CT was performed at ten minutes and 60 minutes after injection, respectively. Images were evaluated by three nuclear medicine doctors based on: 1) visual analysis of the three methods based on tracer uptake model, and PET images attenuation-corrected with CT and those not attenuation-corrected with CT were analyzed, respectively; and 2) semi-quantitative analysis of PET/CT: maximum standardized uptake value (SUVmax) of lesions, SUVmax of the lesion/SUVmean of the normal bone, and SUVmax of the lesion/SUVmean of the normal muscle. The final diagnosis was based on the clinical and intraoperative findings, and histopathological and microbiological examinations.
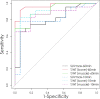
Results: Overall, 23 and 16 patients were diagnosed with PJI and AL, respectively. The sensitivity and specificity of three-phase bone scan and SPECT/CT were 100% and 62.5%, 82.6%, and 100%, respectively. Attenuation correction (AC) at 60 minutes and non-AC at 60 minutes of PET/CT had the same highest sensitivity and specificity (91.3% and 100%), and AC at 60 minutes combined with SPECT/CT could improve the diagnostic efficiency (sensitivity = 95.7%). Diagnostic efficacy of the SUVmax was low (area under the curve (AUC) of ten minutes and 60 minutes was 0.814 and 0.806, respectively), and SUVmax of the lesion/SUVmean of the normal bone at 60 minutes was the best semi-quantitative parameter (AUC = 0.969).
Conclusion: 68Ga-citrate showed the potential to differentiate PJI from AL, and visual analysis based on uptake pattern of tracer was reliable. The visual analysis method of AC at 60 minutes, combined with 99mTc-MDP SPECT/CT, could improve the sensitivity from 91.3% to 95.7%. In addition, a major limitation of our study was that it had a limited sample size, and more detailed studies with a larger sample size are warranted. Cite this article: Bone Joint Res 2022;11(6):398-408.
Keywords: 68Ga-citrate; 99mTc-MDP; Aseptic loosening; PET/CT; Periprosthetic joint infection; aseptic loosening; bisphosphonates; bone scan; hip; joint replacement surgery; knee; lesions; periprosthetic joint infection (PJI); positron emission tomography; single-photon emission computed tomography.
Figures