Applications of Chitosan in Surgical and Post-Surgical Materials
- PMID: 35736199
- PMCID: PMC9228111
- DOI: 10.3390/md20060396
Applications of Chitosan in Surgical and Post-Surgical Materials
Abstract
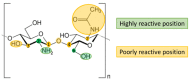
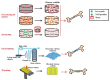
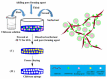
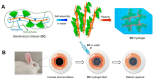
The continuous advances in surgical procedures require continuous research regarding materials with surgical applications. Biopolymers are widely studied since they usually provide a biocompatible, biodegradable, and non-toxic material. Among them, chitosan is a promising material for the development of formulations and devices with surgical applications due to its intrinsic bacteriostatic, fungistatic, hemostatic, and analgesic properties. A wide range of products has been manufactured with this polymer, including scaffolds, sponges, hydrogels, meshes, membranes, sutures, fibers, and nanoparticles. The growing interest of researchers in the use of chitosan-based materials for tissue regeneration is obvious due to extensive research in the application of chitosan for the regeneration of bone, nervous tissue, cartilage, and soft tissues. Chitosan can serve as a substance for the administration of cell-growth promoters, as well as a support for cellular growth. Another interesting application of chitosan is hemostasis control, with remarkable results in studies comparing the use of chitosan-based dressings with traditional cotton gauzes. In addition, chitosan-based or chitosan-coated surgical materials provide the formulation with antimicrobial activity that has been highly appreciated not only in dressings but also for surgical sutures or meshes.
Keywords: bleeding control; bone regeneration; hemostasis; hydrogels; scaffolds; soft tissue; sponges; sutures; tissue regeneration; viscosupplementation.
Conflict of interest statement
The authors declare no conflict of interest.
Figures



Similar articles
-
Polysaccharide Based Hemostatic Strategy for Ultrarapid Hemostasis.Macromol Biosci. 2020 Apr;20(4):e1900370. doi: 10.1002/mabi.201900370. Epub 2020 Feb 18. Macromol Biosci. 2020. PMID: 32068950 Review.
-
Using absorbable chitosan hemostatic sponges as a promising surgical dressing.Int J Biol Macromol. 2015 Apr;75:322-9. doi: 10.1016/j.ijbiomac.2015.01.049. Epub 2015 Feb 4. Int J Biol Macromol. 2015. PMID: 25661881
-
Effectiveness of chitosan scaffold in skin, bone and cartilage healing.Int J Biol Macromol. 2017 Nov;104(Pt A):1003-1011. doi: 10.1016/j.ijbiomac.2017.06.124. Epub 2017 Jul 3. Int J Biol Macromol. 2017. PMID: 28684351 Review.
-
Chitosan-Based Composite Materials for Prospective Hemostatic Applications.Mar Drugs. 2018 Aug 4;16(8):273. doi: 10.3390/md16080273. Mar Drugs. 2018. PMID: 30081571 Free PMC article. Review.
-
Applicatoin of chitosan-based hydrogel in oral tissue engineering.Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2023 Jan 28;48(1):138-147. doi: 10.11817/j.issn.1672-7347.2023.220370. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2023. PMID: 36935187 Free PMC article. Chinese, English.
Cited by
-
Biomaterials Based on Chitosan and Polyvinyl Alcohol as a Drug Delivery System with Wound-Healing Effects.Gels. 2023 Feb 1;9(2):122. doi: 10.3390/gels9020122. Gels. 2023. PMID: 36826292 Free PMC article.
-
Evaluation of Chitosan-Based Axiostat as Hemostatic Dressing for Endovascular Procedures in Patients with Leriche Syndrome on Anticoagulant Therapy.Pharmaceuticals (Basel). 2025 Apr 16;18(4):584. doi: 10.3390/ph18040584. Pharmaceuticals (Basel). 2025. PMID: 40284019 Free PMC article.
-
Thymol as a Component of Chitosan Systems-Several New Applications in Medicine: A Comprehensive Review.Plants (Basel). 2024 Jan 25;13(3):362. doi: 10.3390/plants13030362. Plants (Basel). 2024. PMID: 38337895 Free PMC article. Review.
-
Therapeutic functions of medical implants from various material categories with integrated biomacromolecular systems.Front Bioeng Biotechnol. 2025 Jan 10;12:1509397. doi: 10.3389/fbioe.2024.1509397. eCollection 2024. Front Bioeng Biotechnol. 2025. PMID: 39867472 Free PMC article. Review.
-
Chitosan Hemostatic Dressings: Properties and Surgical Applications.Polymers (Basel). 2024 Jun 22;16(13):1770. doi: 10.3390/polym16131770. Polymers (Basel). 2024. PMID: 39000626 Free PMC article. Review.
References
-
- Global Surgery 2030. The Lancet Comission on Global Surgery. [(accessed on 13 May 2022)]. Available online: https://b6cf2cfd-eb09-4859-92a9-a8f002c3bcef.filesusr.com/ugd/346076_713....
-
- Scalise A., Calamita R., Tartaglione C., Pierangeli M., Bolletta E., Gioacchini M., Gesuita R., Di Benedetto G. Improving wound healing and preventing surgical site complications of closed surgical incisions: A possible role of Incisional Negative Pressure Wound Therapy. A systematic review of the literature. Int. Wound J. 2015;13:1260–1281. doi: 10.1111/iwj.12492. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

