Conflicting Aims and Values in the Application of Smart Sensors in Geriatric Rehabilitation: Ethical Analysis
- PMID: 35737429
- PMCID: PMC9264133
- DOI: 10.2196/32910
Conflicting Aims and Values in the Application of Smart Sensors in Geriatric Rehabilitation: Ethical Analysis
Abstract
Background: Smart sensors have been developed as diagnostic tools for rehabilitation to cover an increasing number of geriatric patients. They promise to enable an objective assessment of complex movement patterns.
Objective: This research aimed to identify and analyze the conflicting ethical values associated with smart sensors in geriatric rehabilitation and provide ethical guidance on the best use of smart sensors to all stakeholders, including technology developers, health professionals, patients, and health authorities.
Methods: On the basis of a systematic literature search of the scientific databases PubMed and ScienceDirect, we conducted a qualitative document analysis to identify evidence-based practical implications of ethical relevance. We included 33 articles in the analysis. The practical implications were extracted inductively. Finally, we carried out an ethical analysis based on the 4 principles of biomedical ethics: autonomy, beneficence, nonmaleficence, and justice. The results are reported in categories based on these 4 principles.
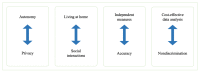
Results: We identified 8 conflicting aims for using smart sensors. Gains in autonomy come at the cost of patient privacy. Smart sensors at home increase the independence of patients but may reduce social interactions. Independent measurements performed by patients may result in lower diagnostic accuracy. Although smart sensors could provide cost-effective and high-quality diagnostics for most patients, minorities could end up with suboptimal treatment owing to their underrepresentation in training data and studies. This could lead to algorithmic biases that would not be recognized by medical professionals when treating patients.
Conclusions: The application of smart sensors has the potential to improve the rehabilitation of geriatric patients in several ways. It is important that patients do not have to choose between autonomy and privacy and are well informed about the insights that can be gained from the data. Smart sensors should support and not replace interactions with medical professionals. Patients and medical professionals should be educated about the correct application and the limitations of smart sensors. Smart sensors should include an adequate representation of minorities in their training data and should be covered by health insurance to guarantee fair access.
Keywords: access to health care; autonomy; ethics; justice; machine learning; older adults; personal data; rehabilitation; smart sensor; wearable.
©Christopher Predel, Cristian Timmermann, Frank Ursin, Marcin Orzechowski, Timo Ropinski, Florian Steger. Originally published in JMIR mHealth and uHealth (https://mhealth.jmir.org), 23.06.2022.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures
References
-
- Polhemus AM, Bergquist R, Bosch de Basea M, Brittain G, Buttery SC, Chynkiamis N, Dalla Costa G, Delgado Ortiz L, Demeyer H, Emmert K, Garcia Aymerich J, Gassner H, Hansen C, Hopkinson N, Klucken J, Kluge F, Koch S, Leocani L, Maetzler W, Micó-Amigo ME, Mikolaizak AS, Piraino P, Salis F, Schlenstedt C, Schwickert L, Scott K, Sharrack B, Taraldsen K, Troosters T, Vereijken B, Vogiatzis I, Yarnall A, Mazza C, Becker C, Rochester L, Puhan MA, Frei A. Walking-related digital mobility outcomes as clinical trial endpoint measures: protocol for a scoping review. BMJ Open. 2020 Jul 19;10(7):e038704. doi: 10.1136/bmjopen-2020-038704. https://bmjopen.bmj.com/lookup/pmidlookup?view=long&pmid=32690539 bmjopen-2020-038704 - DOI - PMC - PubMed
-
- Patel S, Park H, Bonato P, Chan L, Rodgers M. A review of wearable sensors and systems with application in rehabilitation. J Neuroeng Rehabil. 2012 Apr 20;9:21. doi: 10.1186/1743-0003-9-21. https://jneuroengrehab.biomedcentral.com/articles/10.1186/1743-0003-9-21 1743-0003-9-21 - DOI - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources