Manual Therapy Facilitates Homeostatic Adaptation to Bone Microstructural Declines Induced by a Rat Model of Repetitive Forceful Task
- PMID: 35743030
- PMCID: PMC9223642
- DOI: 10.3390/ijms23126586
Manual Therapy Facilitates Homeostatic Adaptation to Bone Microstructural Declines Induced by a Rat Model of Repetitive Forceful Task
Abstract
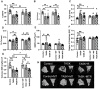
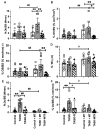
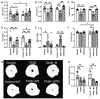
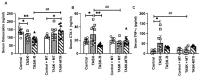
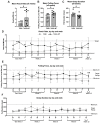
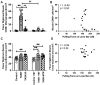
The effectiveness of manual therapy in reducing the catabolic effects of performing repetitive intensive force tasks on bones has not been reported. We examined if manual therapy could reduce radial bone microstructural declines in adult female Sprague-Dawley rats performing a 12-week high-repetition and high-force task, with or without simultaneous manual therapy to forelimbs. Additional rats were provided 6 weeks of rest after task cessation, with or without manual therapy. The control rats were untreated or received manual therapy for 12 weeks. The untreated TASK rats showed increased catabolic indices in the radius (decreased trabecular bone volume and numbers, increased osteoclasts in these trabeculae, and mid-diaphyseal cortical bone thinning) and increased serum CTX-1, TNF-α, and muscle macrophages. In contrast, the TASK rats receiving manual therapy showed increased radial bone anabolism (increased trabecular bone volume and osteoblast numbers, decreased osteoclast numbers, and increased mid-diaphyseal total area and periosteal perimeter) and increased serum TNF-α and muscle macrophages. Rest, with or without manual therapy, improved the trabecular thickness and mid-diaphyseal cortical bone attributes but not the mineral density. Thus, preventive manual therapy reduced the net radial bone catabolism by increasing osteogenesis, while rest, with or without manual therapy, was less effective.
Keywords: massage therapy; osteoblast; osteoclasts; overuse injury; repetitive motion disorder; work-related musculoskeletal disorders.
Conflict of interest statement
The authors declare no conflict of interest. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Figures

References
-
- Panush R.S. Occupational and Recreational Musculoskeletal Disorders. In: Firestein G.S., Budd R.C., Gariel S.E., McInnes I.B., O’Dell J.R., editors. Kelley and Firestein’s Textbook of Rheumatology. Elsevier; Philadelpia, PA, USA: 2017.
-
- NIOSH National Manufacturing Agenda—June 2010. [(accessed on 23 October 2011)]; Available online: http://www.cdc.gov/niosh/nora/comment/agendas/manuf/
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

