Prevalence of tuberculosis (TB), including multi-drug-resistant and extensively-drug-resistant TB, and association with occupation in adults at Sirindhorn Hospital, Bangkok
- PMID: 35757070
- PMCID: PMC9216408
- DOI: 10.1016/j.ijregi.2022.01.004
Prevalence of tuberculosis (TB), including multi-drug-resistant and extensively-drug-resistant TB, and association with occupation in adults at Sirindhorn Hospital, Bangkok
Abstract
Background: Tuberculosis (TB) affects both child and adult populations worldwide.
Objectives: This retrospective study was conducted to survey the prevalence of TB and its association with patient occupation in an adult population diagnosed with TB at Sirindhorn Hospital in 2018.
Methods: Data were extracted from the medical records of 186 patients with TB, and prevalence and odds ratios were calculated.
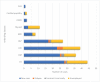
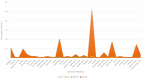
Results: Pulmonary (83.3%) and extrapulmonary TB (17.7%) were observed among the cases. Overall, 70.4% of cases were male and 29.6% were female. Mono-drug-resistant TB, multi-drug-resistant TB and extensively-drug-resistant TB were observed in 2.72%, 4.1% and 0.68% of cases, respectively. Although not statistically significant, individuals with comorbidities had a 2.16-fold [95% confidence interval (CI) 0.33-13.98] higher risk of TB compared with those without comorbidities. Unemployed patients with TB were 4-fold (95% CI 0.82-19.42) more likely to have hypertension than employed patients or traders. The risk of TB among patients with human immunodeficiency virus (HIV) infection was 2.22-fold (95% CI 0.93-5.31) higher among females compared with males, and relapsed patients had a 0.92-fold (95% CI 0.19-4.47) lower risk of HIV infection as a comorbidity compared with new TB cases.
Conclusion: Patient occupation could play a role in the prevalence of TB among communities. The highest prevalence of TB was observed among unemployed subjects, and unemployed patients with TB were more likely to have hypertension as a comorbidity. Mapping the zones/areas of residence for patients with TB could assist in identifying TB hot spots, and could improve understanding of the drivers of the high TB burden and associated socio-economic factors. More studies are required to further understand the drivers that are leading to the high TB burden and the risks posed by occupations.
Keywords: Diabetes; Hypertension; Occupation (livelihood); Pulmonary tuberculosis; Socio-economic factors.
© 2022 The Author(s).
Figures

References
-
- Dean AS, Zignol M, Falzon D, Getahun H, Floyd K. HIV and multidrug-resistant tuberculosis: overlapping epidemics. Eur Respir J. 2014;44:251–254. - PubMed
LinkOut - more resources
Full Text Sources

