Tooth root resorption: A review
- PMID: 35759366
- PMCID: PMC10358711
- DOI: 10.1177/00368504221109217
Tooth root resorption: A review
Abstract
Tooth root resorption is multifactorial, leading to progressive destruction and eventual loss of tooth root dentin and cement. There are internal and external types of root resorption, each having its variety. The etiology and pathogenesis of tooth root resorption are poorly understood, and the most significant etiological factors are trauma, pulpal infection, tooth bleaching, and orthodontic treatment. Tooth root resorption is primarily asymptomatic; thus, it is revealed accidentally by radiographic examination. Progressive clinical manifestations are pain, tooth discoloration, tooth mobility, and other conditions. Awareness of the causes and risk factors allowing tooth root resorption, and regular radiographic examination, in case of necessity, make it possible to reveal resorption at an early stage and to prevent its further development. Thus, the aim of this study is to present etiopathogenesis, a clinical course, and diagnostic peculiarities of internal and external types of tooth root resorption, enabling practicing dentists to timely diagnose root resorption and take appropriate measures to avoid further complications. Within the limitation of this review, even though the etiopathogenesis of tooth root resorption is yet not fully understood, it is suggested that the etiological factors fall into two groups (endogenic and exogenic) to enhance further understanding of the possible causes and mechanisms of root resorption and allow practitioners to monitor high-risk patients and make timely diagnoses. Moreover, radiographic examination and CBCT are indispensable for the diagnosis of root resorption.
Keywords: Root resorption; dental trauma; external resorption; internal resorption; orthodontic force; resorption classification; resorption diagnosis; resorption etiology; resorption pathogenesis.
Conflict of interest statement
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures

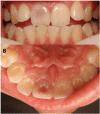




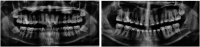
References
-
- Brezniak N, Wasserstein A. Orthodontitis: “the inflammation behind tooth movement and orthodontic root resorption. In: Shroff B. (ed) Biology of orthodontic tooth movement: current concepts and applications in orthodontic practice. Switzerland: Springer International Publishing, 2016, pp.67–101.
-
- Al-Qawasmi RA, Hartsfield JK, Jr., et al.Genetic predisposition to external apical root resorption. American Journal of Orthodontics & Dentofacial Orthopedics 2003; 123: 242–252. - PubMed
-
- Abuara A. Biomechanical aspects of external root resorption in orthodontic therapy. Med Oral Patol Oral Cir Bucal 2007; 12: E610–E613. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

