GASTRIC TWIST AFTER SLEEVE GASTRECTOMY: A PROPOSAL FOR ENDOSCOPIC CLASSIFICATION
- PMID: 35766610
- PMCID: PMC9254382
- DOI: 10.1590/0102-672020210002e1665
GASTRIC TWIST AFTER SLEEVE GASTRECTOMY: A PROPOSAL FOR ENDOSCOPIC CLASSIFICATION
Abstract
Objective: The twisting of the gastric tube is one of the main causes of persistent reflux and food intolerance after sleeve gastrectomy (SG). To date, there is no classification for gastric twist after SG. This study aimed to propose an endoscopic classification for this condition and outline the clinical profile of these patients with sleeve gastrectomy.
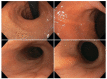
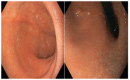
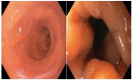
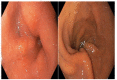
Methods: Patients in the postoperative period of SG presenting endoscopic findings of gastric twist were included. All patients underwent an esophagogastroduodenoscopy 12 months after SG. The classification proposed consists of three degrees: degree I: mild rotation of the staple line without relevant shrinkage of the gastric lumen; degree II: moderate rotation of the staple line, leading to a focal area of fixed narrowing that requires additional maneuvers for its transposition; and degree III: severe rotation of the staple line leading to stenosis, with increased difficulty for transposition or complete blockage.
Results: Out of 2,723 patients who underwent SG, 45 (1.6%) presented gastric twist. Most patients were female (85%), with mean age of 39±10.4 years. In all, 41 (91.1%) presented degree I, 3 (6.7%) presented degree II, and 1 (2.2%) had degree III. Most patients were asymptomatic (n=26). Vomiting was the most prevalent symptom (15.5%). Statistically significant correlation of twisting degrees was not observed for both the presence of symptoms and the degrees of esophagitis.
Conclusion: Gastric twist after SG is rare, with generally mild and asymptomatic presentation. The endoscopic classification was not statistically related to clinical presentation but set the ground for further analysis.
A torção do tubo gástrico ou twist é uma das principais causas de refluxo persistente e intolerância alimentar após a gastrectomia vertical (GV). Até o momento, não há uma classificação proposta para a torção gástrica após GV.
OBJETIVO:: Propor uma classificação endoscópica para essa condição e descrever o perfil clínico desses pacientes.
MÉTODOS:: Pacientes no pós-operatório de GV apresentando achados endoscópicos de twist foram incluídos. Os pacientes foram submetidos a uma esofagogastroduodenoscopia 12 meses após a cirurgia. A classificação consiste em três graus. Grau I: rotação leve da linha de grampos, sem redução relevante do lúmen gástrico. Grau II: rotação moderada da linha de grampos, levando a uma área de estreitamento focal que requer manobras adicionais para a progressão do aparelho. Grau III: rotação severa da linha de grampos, levando à estenose, com grande dificuldade de progressão ou obstrução completa.
RESULTADOS:: Dos 2.723 pacientes que foram submetidos à GV, 45 (1,6%) apresentaram twist. A maioria dos pacientes era do sex feminino (85%), com idade média de 39±10.4 anos. Quarenta e um (91,1%) apresentaram twist grau I, 3 (6,7%) apresentaram twist grau II e apenas 1 (2,2%) apresentou twist grau III. A maioria dos pacientes eram assintomáticos (n=26). O sintoma mais prevalente foi vômito (15,5%). Não foi observada correlação estatisticamente significante entre o grau de twist e a presença de sintomas ou esofagite.
CONCLUSÃO:: Twist após GV é raro e geralmente assintomático. A classificação endoscópica proposta não foi estatisticamente relacionada com apresentação clínica, porém estabelece um referencial para análises futuras.
Conflict of interest statement
Conflict of interest: None.
Figures
Similar articles
-
The Impact of the Gastric Twist on Esophagitis Progression After Sleeve Gastrectomy: Mid-Term Endoscopic Findings.Obes Surg. 2020 Nov;30(11):4452-4458. doi: 10.1007/s11695-020-04838-0. Epub 2020 Jul 14. Obes Surg. 2020. PMID: 32661958
-
Incidence of Abnormalities of the Gastric Tube Following Sleeve Gastrectomy and Its Role on Esophagitis Progression.Obes Surg. 2023 Jan;33(1):263-267. doi: 10.1007/s11695-022-06375-4. Epub 2022 Dec 3. Obes Surg. 2023. PMID: 36460942
-
Gastroesophageal reflux disease and Barrett's esophagus after laparoscopic sleeve gastrectomy: a possible, underestimated long-term complication.Surg Obes Relat Dis. 2017 Apr;13(4):568-574. doi: 10.1016/j.soard.2016.11.029. Epub 2016 Dec 9. Surg Obes Relat Dis. 2017. PMID: 28089434
-
Effect of Concomitant Laparoscopic Sleeve Gastrectomy and Hiatal Hernia Repair on Gastroesophageal Reflux Disease in Patients with Obesity: a Systematic Review and Meta-analysis.Obes Surg. 2021 Sep;31(9):3905-3918. doi: 10.1007/s11695-021-05545-0. Epub 2021 Jul 12. Obes Surg. 2021. PMID: 34254259
-
Is Routine Preoperative Esophagogastroduodenoscopy Screening Necessary Prior to Laparoscopic Sleeve Gastrectomy? Review of 1555 Cases and Comparison with Current Literature.Obes Surg. 2018 Jan;28(1):52-60. doi: 10.1007/s11695-017-2813-4. Obes Surg. 2018. PMID: 28685362 Review.
Cited by
-
The Efficacy and Safety of Endoscopic Balloon Dilatation in the Treatment of Functional Post-Sleeve-Gastrectomy Stenosis.Medicina (Kaunas). 2024 May 19;60(5):833. doi: 10.3390/medicina60050833. Medicina (Kaunas). 2024. PMID: 38793016 Free PMC article.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

